|
Page 4 of 9
|
Print this Chapter ( K) |
Chapter 10: Retina
RETINAL VASCULAR DISEASES
DIABETIC RETINOPATHY
Diabetic retinopathy is one of the leading causes of blindness in the Western world. The view that chronic hyperglycemia of diabetes mellitus is the major determinant of diabetic retinopathy is supported by the observation that retinopathy in young people with type I (insulin-dependent) diabetes does not occur for at least 3-5 years after the onset of this systemic disease. Similar results have been obtained for type II (non-insulin-dependent) diabetes, but in such patients the time of onset and therefore the duration of disease are more difficult to determine precisely. It is recommended that patients with type I diabetes mellitus be referred for ophthalmologic examination within 3 years after diagnosis and reexamined on at least an annual basis. Type II diabetic patients should be referred for ophthalmologic examination at the time of diagnosis and reexamined at least annually. As diabetic retinopathy can become particularly aggressive during pregnancy, any diabetic woman who becomes pregnant should be examined by an ophthalmologist in the first trimester and at least every 3 months thereafter until parturition.
In terms of both prognosis and treatment, it is useful to divide diabetic retinopathy into nonproliferative and proliferative categories. The prevalence of proliferative retinopathy in type I diabetics with 15 years of systemic disease is 50%. While the prevalence of proliferative disease at 15 years is much less in type II diabetics, the prevalence of macular edema as a function of the duration of systemic disease is the same in both groups.
1. NONPROLIFERATIVE DIABETIC RETINOPATHY
Diabetic retinopathy is a progressive microangiopathy characterized by small vessel damage and occlusion. The earliest pathologic changes are thickening of the capillary endothelial basement membrane and reduction of the number of pericytes. Background diabetic retinopathy is a clinical reflection of the hyperpermeability and incompetence of involved vessels. The capillaries develop tiny dot-like outpouchings called microaneurysms, while the retinal veins become dilated and tortuous (Figure 10-20).
Multiple hemorrhages may appear throughout different levels of the retina. Flame-shaped hemorrhages are so shaped because of their location within the horizontally oriented nerve fiber layer, while dot and blot hemorrhages are in the deeper retina, where cells and axons are vertically oriented.
Macular edema is the most frequent cause of visual loss among patients with background diabetic retinopathy. The edema is caused primarily by a breakdown of the inner blood-retinal barrier at the level of the retinal capillary endothelium, allowing leakage of fluid and plasma constituents into the surrounding retina. The edema may be focal or diffuse and appears clinically as thickened, cloudy retina with associated microaneurysms and intraretinal exudate. Circinate zones of yellow, lipid-rich exudate may form around clusters of microaneurysms and are most frequently centered in the temporal portion of the macula. While the prevalence of macular edema is 10% in the diabetic population as a whole, there is a dramatic increase in prevalence in eyes with more severe retinopathy.
With progressive microvascular occlusion, signs of increasing ischemia may be superimposed on the picture of background retinopathy and produce the clinical picture of preproliferative diabetic retinopathy. The most typical findings here are multiple cotton-wool spots, beading of the retinal veins, and irregular segmental dilation of the retinal capillary bed (intraretinal microvascular abnormalities). Closure of retinal capillaries surrounding the foveal avascular zone may cause significant ischemia, manifest clinically by the presence of large dark retinal hemorrhages and small thread-like macular arterioles. Eyes with macular edema and significant ischemia have a poorer visual prognosis-with or without laser treatment-than eyes with edema and relatively good perfusion.
The visual and electrophysiologic dysfunctions associated with diabetes probably result from the local vascular abnormalities and the systemic metabolic effects of the disease to which the retina is subjected. A characteristic blue-yellow color vision abnormality develops, and hue discrimination may be impaired. Contrast sensitivity may be reduced in patients, even in the presence of normal visual acuity. Visual field testing may show relative scotomas corresponding to areas of retinal edema and nonperfusion, and abnormalities in dark adaptation have also been described. Electroretinographic abnormalities bear a relationship to the severity of retinopathy and may aid in predicting progression of retinopathy. Fluorescein angiography is invaluable in defining the microvascular abnormalities of diabetic retinopathy (Figures 10-21 and 10-22). Large filling defects of capillary beds-"capillary nonperfusion"-show the extent of retinal ischemia (Figure 10-23) and are usually most prominent in the midperiphery. The fluorescein leakage associated with retinal edema may assume the petaloid configuration of cystoid macular edema or may be diffuse. Other fluorescein abnormalities include vascular loops and intraretinal shunts. The focus of treatment in patients with nonproliferative diabetic retinopathy and no macular edema is treatment of hyperglycemia and intercurrent systemic disease. A controlled clinical trial has shown that aldose reductase inhibitor therapy does not prevent progression of diabetic retinopathy. Focal argon laser treatment of discrete points of retinal leakage in patients with clinically significant macular edema, principally defined as thickening of the retina at or within 500 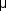 m of the center of the macula, reduces the risk of visual loss and increases the likelihood of visual improvement (see Chapter 24). Eyes with diabetic macular edema that is not clinically significant should usually be monitored closely without laser treatment. Since macular edema may be present with little or no change in visual acuity and requires slitlamp biomicroscopic retinal examination for full evaluation, primary health care providers should recognize the importance of prompt and early referral of diabetic patients to the ophthalmologist.
m of the center of the macula, reduces the risk of visual loss and increases the likelihood of visual improvement (see Chapter 24). Eyes with diabetic macular edema that is not clinically significant should usually be monitored closely without laser treatment. Since macular edema may be present with little or no change in visual acuity and requires slitlamp biomicroscopic retinal examination for full evaluation, primary health care providers should recognize the importance of prompt and early referral of diabetic patients to the ophthalmologist.
2. PROLIFERATIVE DIABETIC RETINOPATHY
The most severe ocular complications of diabetes mellitus are associated with proliferative diabetic retinopathy. Progressive retinal ischemia eventually stimulates the formation of delicate new vessels that leak serum proteins (and fluorescein) profusely. Neovascularization is frequently located on the surface of the disk and at the posterior edge of the peripheral zones of "nonperfusion" (Figures 10-24 and 10-25). Iris neovascularization, or rubeosis iridis, can also result.
The fragile new vessels proliferate onto the posterior face of the vitreous and become elevated once the vitreous starts to contract away from the retina. If the vessels bleed (Figure 10-26), massive vitreous hemorrhage may cause sudden visual loss. Eyes in which posterior vitreous detachment is complete are at less risk of developing neovascularization and vitreous hemorrhage. In eyes with proliferative diabetic retinopathy and persistent vitreoretinal adhesions, elevated neovascular fronds may undergo fibrous change and form tight fibrovascular bands that tug on the retina and exert continued vitreous contraction. This can cause either a progressive traction retinal detachment or, if a retinal tear is produced, rhegmatogenous retinal detachment. The retinal detachment may be heralded or concealed by vitreous hemorrhage. When vitreous contraction is complete in these eyes, proliferative retinopathy tends to enter the burned-out or "involutional" stage.
Treatment
Argon laser panretinal photocoagulation is usually indicated in proliferative diabetic retinopathy. Patients at greatest risk of significant visual loss are those with preretinal or vitreous hemorrhage or neovascularization of the disk. Panretinal photocoagulation can significantly reduce the chance of massive vitreous hemorrhage and retinal detachment in these patients by causing the regression and, in some cases, the disappearance of new vessels. The technique involves scattering up to several thousand regularly spaced laser burns throughout the retina, sparing the central region bordered by the disk and the major temporal vascular arcades (Chapter 24). Although the mechanism is not precisely understood, panretinal photocoagulation presumably works by reducing the angiogenic stimulus from ischemic retina.
The role of vitreoretinal surgery in proliferative diabetic eye disease continues to evolve. Conservative management of monocular vision impairing diabetic vitreous hemorrhage in the binocular patient had been to allow spontaneous resolution over the course of several months. The results of a 4-year study designed to assess the role of early vitrectomy for severe vitreous hemorrhage and proliferative diabetic retinopathy support this surgery as a means by which good vision may be restored or maintained. The role of vitreoretinal surgery in the treatment of diabetic traction retinal detachment is described elsewhere in this chapter.
CENTRAL RETINAL ARTERY OCCLUSION
The patient with central retinal artery occlusion routinely relates a history of painless catastrophic visual loss occurring over a period of seconds; antecedent transient visual loss (amaurosis fugax) may be reported. The visual acuity ranges between counting fingers and light perception in 90% of eyes at the time of initial examination. An afferent pupillary defect can appear within seconds after retinal arterial obstruction, preceding the fundus abnormalities by an hour.
Ophthalmoscopically, the superficial retina becomes opacified except in the foveola, where a cherry-red spot is evident (Figure 10-27). The cherry-red spot is pigment of the choroid and retinal pigment epithelium viewed through the extremely thin overlying foveolar retina and contrasted with the thicker and translucent perifoveolar retina. Twenty-five percent of eyes with central retinal artery occlusion have cilioretinal arteries that spare macular retina and may preserve some central visual acuity. Clinically, the retinal opacification resolves within 4-6 weeks, leaving a pale optic disk as the major ocular finding. In older patients, giant cell arteritis must be excluded and if necessary treated immediately with high doses of systemic corticosteroids. Other causes of central retinal artery occlusion are arteriosclerosis and emboli from carotid or cardiac sources. These are discussed further in Chapter 15.
Treatment
Because irreversible retinal damage has been shown to occur after 90 minutes of complete central retinal artery occlusion in the subhuman primate model, precious little time is available in which to begin therapy. Anterior chamber paracentesis can be employed in order to decrease intraocular pressure and increase retinal perfusion. This is particularly indicated in embolic central retinal artery occlusion. Intravenous acetazolamide has been used to decrease intraocular pressure, and an inhaled oxygen-carbon dioxide mixture has been employed to induce retinal vasodilation and increase the PO2 at the retinal surface. Direct infusion of a thrombolytic agent into the ophthalmic artery can result in recovery of vision. It must be performed within 8 hours after onset of the central retinal artery occlusion, requires specific radiologic expertise, and there is a risk of cerebral infarction. Systemic anticoagulants are generally not employed.
BRANCH RETINAL ARTERY OCCLUSION
Branch retinal artery occlusion usually presents with sudden loss of visual field and with reduction in visual acuity if the fovea is involved. Fundus signs of retinal edema with associated cotton-wool spots are limited to the area of retina supplied by the occluded vessel. Embolic causes are proportionately more common than in central retinal artery occlusion, and emboli are frequently identified on clinical examination (see Chapter 15). Migraine, oral contraceptive use, and vasculitis must also be considered.
CENTRAL RETINAL VEIN OCCLUSION
Central retinal vein occlusion is a common and easily diagnosed retinal vascular disorder with potentially blinding complications. The patient presents with sudden painless loss of vision. The clinical appearance varies from a few small scattered retinal hemorrhages and cotton-wool spots (Figure 10-28) to a marked hemorrhagic appearance with both deep and superficial retinal hemorrhage, which may rarely break through into the vitreous cavity. Most patients who develop the disease are over 50 years of age, and more than half have associated cardiovascular disease. Predisposing factors and their investigation are discussed in Chapter 15. Chronic open-angle glaucoma should always be excluded (see Chapter 11).
The two major complications associated with central retinal vein occlusion are reduced vision from macular edema and neovascular glaucoma secondary to iris neovascularization. Macular dysfunction occurs in almost all eyes with central vein occlusion. Although some eyes will show spontaneous improvement, most eyes will have persistent decreased central vision as a result of chronic macular edema. Nearly one-third of eyes with central retinal vein occlusion show significant retinal capillary nonperfusion on fluorescein angiography; one-half of these eyes will develop neovascular glaucoma.
Treatment
Careful follow-up evaluation is warranted, and prompt panretinal laser photocoagulation is recommended for eyes that develop anterior segment neovascularization. No treatment for macular edema, including grid pattern photocoagulation, has proved effective to date.
BRANCH RETINAL VEIN OCCLUSION
Branch retinal vein occlusion presents as sudden unilateral vision loss with segmentally distributed intraretinal hemorrhage. The vein occlusion always occurs at the site of an arteriovenous crossing (Figure 10-29), and retinal neovascularization may develop if the occlusion produces an area of retinal capillary nonperfusion that is more than 5 disk diameters in area. Sight-threatening complications of the disease are macular edema, macular ischemia, and vitreous hemorrhage from retinal neovascularization.
Treatment
Once peripheral retinal neovascularization has developed, sectoral laser retinal photocoagulation to the area of ischemic retina reduces the risk of vitreous hemorrhage by one-half. When vision loss due to macular edema persists for several months without spontaneous improvement, grid pattern argon laser macular photocoagulation may be indicated. Anticoagulant therapy has not been shown to be beneficial in either the prevention or the management of branch retinal vein occlusion. Investigation for an underlying systemic cause is discussed in Chapter 15. Important associated ocular diseases are chronic open-angle glaucoma and uveitis secondary to Behçet's syndrome.
RETINAL ARTERIAL MACROANEURYSM
Retinal macroaneurysms are fusiform or round dilations of the retinal arterioles occurring within the first three orders of arteriolar bifurcation. Most cases are unilateral, and the superotemporal artery is the most commonly involved vessel. Two-thirds of patients have associated systemic arterial hypertension.
The most common clinical symptom is loss of central vision as a result of retinal edema, exudation, or hemorrhage. Macroaneurysms may bleed into the subretinal space, into the retina, beneath the internal limiting membrane, or into the vitreous; the "hourglass" hemorrhage is typical and is due to bleeding beneath and anterior to the retina.
Although no clear indication for treatment with laser photocoagulation has been established, laser treatment of the macroaneurysm should be considered if lipid exudate coming from it threatens the fovea.
Page 4 of 9
10.1036/1535-8860.ch10