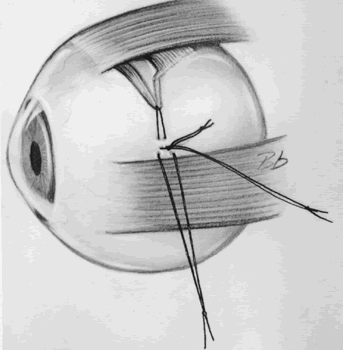
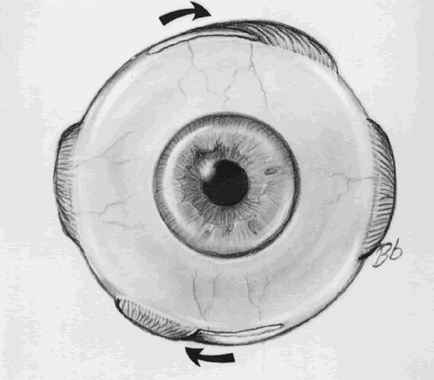
Our preferred method of testing for subjective torsion is the Lancaster red-green test (Fig. 1). This test allows the clinician to evaluate torsion in nine positions of gaze and clearly indicates where torsion is greatest and where vertical deviation is most significant. The test is performed in a darkened room so that no spatial clues in the environment can help in orienting the streaks of red and green light. By convention, a red filter is placed over the right eye and a green filter over the left. The examiner takes the light corresponding to the desired “fixing eye” and shines it on the wall successively in the nine diagnostic positions of gaze. In each position, the patient is asked whether the streak of light is straight or tilted. (We customarily do the test with vertical streaks, in that it is easier for the patient to describe tilt in a vertical streak than a horizontal streak.) If the streak is tilted, the examiner adjusts the light until the patient sees the streak exactly vertically. The patient then superimposes the second streak on the first streak. The examiner records the position and orientation of the streaks to analyze the torsional and vertical components of the deviation in the different fields of gaze (Fig. 2). The absolute horizontal deviation is difficult to judge with this test because of the poor control of accommodation provided by the streaks of colored light. The relative horizontal deviation, however, is reasonably reliable, and is used for judging A or V patterns.
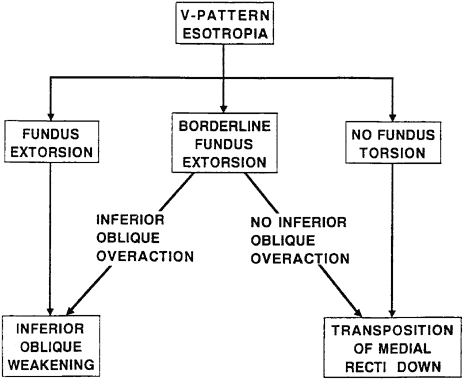
Objective torsion is best assessed by indirect ophthalmoscopy or fundus photography.2,5 For example, in a patient with V-pattern esotropia, the presence of fundus extorsion justifies inferior oblique weakening surgery in addition to horizontal surgery (Fig. 3).
|