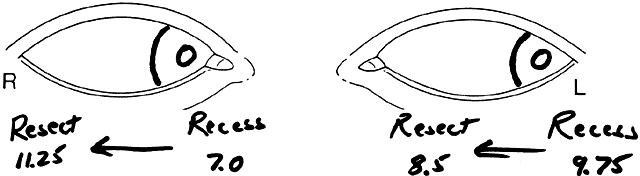BACKGROUND
A subset of patients with congenital nystagmus adopts anomalous head postures. They adopt large face turns and anomalous head postures in the horizontal direction, the vertical direction, or both (Fig. 1). These patients do this to place the eyes in the null position. This position also is known as the zone of minimal intensity of the nystagmus, where the eyes have the smallest amplitude of nystagmus. In this head position, the patient generally achieves the highest level of visual acuity.
|
Anderson1 and Kestenbaum2 were the first to propose surgical procedures for the correction of anomalous horizontal head postures. Their surgical procedures were an attempt to move the null position toward the primary position. Many authors subsequently have addressed the surgical treatment of anomalous head postures associated with congenital nystagmus, most recently Scott,3 Mitchell,4 Biglan,5 and Kraft6 and their coworkers. Such corrective surgery has been shown to be beneficial by eye movement recordings. There is a shift of the null position toward the primary position and a decrease in the intensity of the nystagmus.7–9 In addition, the eye movement recordings demonstrate that the null region is broadened in some patients, allowing a wider angle of best visual acuity compared with the preoperative state.
INDICATIONS
The usual indication for such a surgical procedure is to reduce or eliminate an extreme head posture. Some patients are bothered by neck and back pain from longstanding torticollis. Others achieve the desired reconstruction of eye position, improved visual acuity, and improved stereoacuity.
Preoperative evaluation mirrors that for any patient with nystagmus. A complete ophthalmologic history and examination is needed to elicit the cause of the congenital nystagmus. A pupillary examination for evidence of optic neuropathy or paradoxical pupillary reactions is prudent in the search for a sensory etiology. Electroretinography may be done if there is markedly reduced vision. Neuroimaging is not necessary, unless the nystagmus is acquired or there is optic atrophy. The examiner should observe the patient for at least 10 minutes to be certain that the preferred gaze direction is constant. Congenital nystagmus can present with a periodic, alternating waveform with two different null zones. In such a situation, a Kestenbaum-Anderson type of surgery would be potentially harmful. Four-muscle recession surgery has been suggested for these patients (see later).10
CONTRAINDICATIONS
There are no absolute contraindications. Surgery probably is best deferred until at least age 4 or 5 years. This allows for the surgeon to more accurately determine the operative angle and for the patient to be visually mature.
SURGICAL PROCEDURE
The surgical approach for patients with straight eyes is to move each eye by an equal amount in the direction of the face turn. If there is a strabismus in addition to an anomalous head posture, the surgeon needs to decide whether to correct both in one operation or to pursue correction in two operations.
The approach to the patient with straight eyes and an anomalous head posture follows: The operation should be viewed as one in which the surgeon mechanically moves the eyes in the direction of the face turn (opposite the gaze preference). Thus, a patient in left gaze with a right face turn would undergo a resection of the right lateral rectus, a recession of the right medial rectus, a resection of the left medial rectus, and a recession of the left lateral rectus muscles. The surgeon should take a diagram to the operating room clearly outlining the surgery to be performed (Fig. 2). It is easy during the course of the performance of the surgery to get confused about which muscle undergoes which surgical procedure.
The amounts of surgery to be performed are controversial. The “classic” maximum amount of surgery was formulated by Parks and Mitchell.11,12 Their operation used the guidelines of 5-6-7-8 for the amounts of surgery. These were based on a 5.0-mm medial rectus muscle recession, the maximum medial rectus muscle operation of that period. In my example of a right face turn, the surgery would entail a 5.0-mm recession of the right medial rectus, an 8.0-mm resection of the right lateral rectus, a 7.0-mm recession of the left lateral rectus, and a 6.0-mm resection of the left medial rectus muscle. Notice that the millimeters of surgical correction provided are the same for each eye. Unfortunately, this amount of surgery left many undercorrected patients. Surgeons responded over the ensuing two decades by increasing the amounts of surgery beyond these “maximal amounts.”3,4,13
Before selecting the amount of surgery to be performed, the surgeon must determine the magnitude of the head turn. The patient views a letter chart at distance with the smallest size optotype visible. This helps to establish the maximum deviation. An orthopedic goniometer is one convenient tool for measuring the deviation.4 The head turn is measured in degrees, not prism diopters. The size of the head turn dictates the amount of surgical augmentation. For an anomalous head posture of 20° or less in the horizontal direction, an augmentation of 20% over the 5-6-7-8 guidelines is necessary. Surgical amounts are augmented by 30% for an anomalous position of 21° to 39°. An augmentation of 40% is necessary for head turns of 40° or more. The amounts of horizontal surgery for these head postures are listed in Table 1. Nelson and colleagues suggest that for head postures greater than 45°, an augmentation of 60% is beneficial.13 No other reports lend further substantiation to the efficacy of this marked augmentation.
TABLE 1. Surgical Correction of Anomalous Head Postures*
| Magnitude of head turn (degrees) | 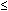 20° 20° | 21–44° | 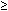 45° 45° |
| Right head turn (move eyes to the right) | |||
| Right medial rectus recession (mm) | 6.0 | 6.5 | 7.0 |
| Right lateral rectus resection (mm) | 9.5 | 10.5 | 11.25 |
| Left medial rectus resection (mm) | 7.25 | 7.75 | 8.5 |
| Left lateral rectus recession (mm) | 8.5 | 9.7 | 9.75 |
| Left head turn (move eyes to the left) | |||
| Right medial rectus resection (mm) | 7.5 | 7.75 | 8.5 |
| Right lateral rectus recession (mm) | 8.5 | 9.0 | 9.75 |
| Left medial rectus recession (mm) | 6.0 | 6.5 | 7.0 |
| Left lateral rectus resection (mm) | 9.5 | 10.5 | 11.25 |
*Surgical amounts rounded to the nearest 0.25 mm.
If the patient has a strabismus in addition to the anomalous head posture, correction of both problems may require one or two operations. When the fixating eye is held in adduction or abduction to allow best acuity, then the appropriate amount of surgery estimated from the table should be performed on the fixating eye. For example, if the right eye is esotropic, fixating in adduction, correction of both the anomalous head posture and the strabismus is possible by recessing the right medial rectus muscle and resecting the right lateral rectus muscle. No surgery is performed on the left eye.
For more complicated combinations of strabismus and anomalous head posture, use of two operations or adjustable sutures should be considered. A surgeon may elect to perform surgery on the fixating eye initially and then perform a second operation on the nonpreferred strabismic eye once the resultant deviation is determined.
RESULTS
The patient who undergoes an augmented Kestenbaum-Anderson operation has two immediate results from surgery. First, there is a marked improvement in the anomalous head posture (Fig. 3). Scott and Kraft3 report that 87% of patients were satisfactorily corrected with the augmented operation (within 15° of straight ahead). Second, every patient has a ductional deficit when the 40% augmentation procedure is performed. The deficit is in the field of action of the recessed muscles. This mechanical ductional deficit is no more a problem for the patient than what the patient experienced preoperatively. Preoperatively, the patient had a functional inability to view in the direction of gaze, and postoperatively, the patient has a mechanical limitation. Each limits the patient in the same way. Every patient should be informed of this risk, and its significance should be carefully explained. This deficit usually is lifelong.
|
In general, the best corrected visual acuity is unchanged with this procedure. However, stereoacuity also has been found to improve in 58% of Biglan's patients.5 Biglan and colleagues5 have shown that this surgical result is not always permanent. Thirteen of their 46 patients met criteria for a second surgery for a recurrence of the anomalous head posture. Scott and Kraft found that only four of seven patients followed for 4 years or longer were stable, whereas three drifted to a larger undercorrection.3
von Noorden reports excellent results from using a modified Anderson operation in which only the recession procedures are performed.14 A 12-mm recession of the lateral rectus is paired with a 10-mm recession of the yoke medial rectus muscle. This procedure would be particularly beneficial if vertical surgery also was needed by a patient.
UNUSUAL INDICATIONS
Although horizontal turns are the most common posture associated with nystagmus, a nystagmus may result in a vertical posture with a chin-down or chin-up posture. Rarely, a nystagmus may induce an anomalous head tilt. For a patient with vertical anomalous head posture, identical surgery is performed on each eye. Parks11 originally recommended 4-mm recessions of the appropriate vertical rectus muscles and 4-mm resection of the antagonist when the anomalous posture exceeds 25°. This procedure generally was inadequate, leading to Park's current recommendations of an 8-mm recession and 8-mm resection for large vertical head posture.12 Roberts and coworkers also note that for a chin-down posture, a large superior rectus muscle recession (8 to 9 mm) combined with inferior oblique recession and anteriorization to the inferior rectus yielded not only improvement in head position, but also better visual acuity in all seven patients who underwent the procedure.15
For patients with an induced torticollis or head tilt, several procedures have been devised. de Decker suggests reproducing the torsional movement of the eyes by using vertical offsets of the horizontal rectus muscles.16 That operation for a left head tilt involves supraplacement of the left lateral rectus muscle, infraplacement of the left medial rectus muscle, infraplacement of the right lateral rectus muscle, and supraplacement of the right medial rectus muscle. Generally, the tendons are shifted one full tendon width, maintaining their normal distance from the limbus. von Noorden and colleagues suggest an alternative approach using the vertical rectus muscles.17 For a head tilt to the right, an excycloduction of the right eye and an incylcloduction of the left eye are needed. To accomplish this, the right superior rectus muscle is transposed nasally, and the right inferior rectus is transposed temporally, causing an excyclorotation of the right eye. In the left eye, a temporal transposition of the left superior rectus muscle and a nasal transposition of the left inferior rectus muscle provide the necessary incycloduction. They report on the outcome of five patients operated with this technique. In four of five patients, the head tilt was eliminated.
COMPLICATIONS
There is a chance of creating a new heterotropia from this surgery. Although Scott and Kraft3 induced no new heterotropias, 1 of 14 patients operated on by Mitchell and colleagues4 did develop a new strabismus. Other complications of the repair of an anomalous head posture are extremely rare. As in any strabismus operation performed on two muscles, anterior segment ischemia is uncommon. It is probably more frequent with two-muscle vertical surgery than with horizontal surgery.18 Induced torsional diplopia from vertical rectus surgery may follow an attempt to correct chin-up and chin-down positions.