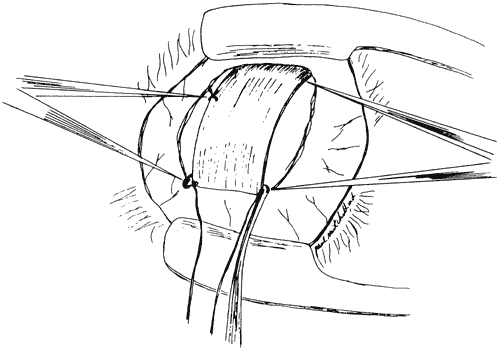
Alan Scott diagrammed the mechanics of Fd.12 He suggested that changing the arc of contact of the muscle with the globe reduces the lever arm formed by the muscle insertion, the center of rotation of the globe, and the origin of the muscle (Fig. 1). Scott's mechanical model suggested that the posterior suture needed to be 10 to 12 mm from the insertion for the medial rectus, 12 to 14 for the superior and lateral recti, and 14 to 16 for the lateral rectus.
|
Kushner measured saccadic velocity after the Fd.13 He expected to find decreased velocity in the field of the operated muscle but did not. He questioned whether the Fd changed the torque active on the muscle as would be suggested by the lever arm theory and also noted that the lever arm theory would not explain the effect of Fd without a recession. He stressed the effect of the amount of muscle contained in the suture and how effectively it was immobilized to explain the clinical effect of the operation.
Clark and colleagues14 examined the theory of the Fd in the context of the extraocular muscle pulleys previously described by Demer and coworkers,15 who described connective tissue sleeves that envelop and position each rectus muscle. Given that the anterior portion of the sleeve overlies the area at the equator where the posterior fixation suture is placed, they suggested that displacement of the pulley sleeve by the posterior suture itself or by extensive sharp dissection posteriorly results in mechanical restriction rather than a reduction in torque during muscle contraction. Their studies that used magnetic resonance imaging (MRI) did not show a change in tangency and thus did not predict a reduction in torque to explain the effect of the Fd. Mechanical restriction created by the Fd would explain the effect of the procedure without simultaneous recession of the muscle. It could also explain the variable results that many researchers have noted.
Regardless of the theory of how it works, there are five points to consider in applying the theory of the Fd in clinical practice and also in evaluating the literature:
- First, it is important to determine how far posteriorly the fixation suture
ought to be placed from the limbus. From the point of view of the
mechanical model, this determines how much the lever arm is shortened, and
thus the farther back such placement is made, the better will the
result be. With the pulley model, extensive posterior orbital dissection
could damage the anterior pulley slings and reduce the desired mechanical
restriction to ocular movement. However, many surgeons try to
put the suture(s) as far back as possible. For example, Biglan (Biglan
AW, personal communication, 2000) has suggested going back 14 mm on
the superior rectus for mild dissociated vertical deviation (DVD), 14.5 mm
for moderate, and 15 mm for severe deviations. H. Eggers (personal
communication, 2000) attempts to go back 15 mm on the medial rectus
for high accomodative:convergence accommodation (AC:A) esotropia. Peterseim
and Buckley16 placed medial rectus sutures an average of 18.3 mm (range, 15 to 20.5 mm). De
Decker4 found that unsuccessful cases on reoperation did not have the suture placed
as far posteriorly as the initial surgeon had claimed.
- Second, the scleral suture (or sutures) needs to be heavy and deep enough
to hold firmly4 and the knots into the muscle have to be tight enough to stay posterior.17 The amount of muscle incorporated in the sutures is important and could
explain variable results.13
- Third, simultaneous recession augments the procedure. Sprague and colleagues5 advocatedrecession of the superior rectus for DVD after disappointing
results without it. Although undercorrection is a problem with DVD, large
simultaneous medial rectus recessions may lead to overcorrections. In
addition, if the posterior suture is placed before the muscle is recessed, the
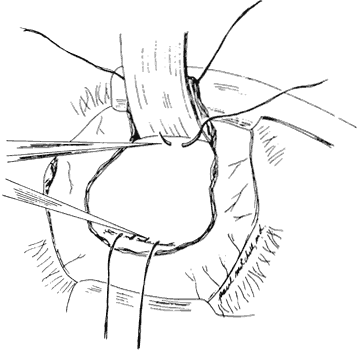
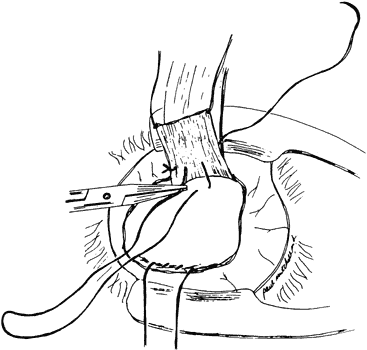
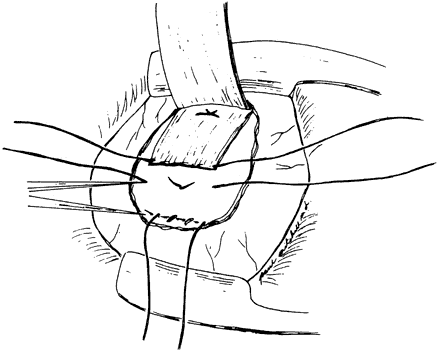
slack in the muscle will be anterior to the posterior attachment. Alan
Scott pointed out that it is more effective to allow the
slack created by the recession to fall behind the posterior suture, in
effect doing the recession first and then placing the posterior suture (Fig. 2).12
- Fourth, previous recession can be augmented with the Fd alone without the
need to recess the muscle further or consider a marginal myotomy.16,18,19
- Fifth, the Fd may weaken the operated muscle by tissue destruction and
scarring.4,7 In rabbit studies, Alio and associates20 found muscle degeneration at the point of posterior fixation as well as
anterior to the insertion. The Fd may lead to muscle stiffening, as
shown by Castenera.21 De Decker found on reoperation that there was adherence of the muscle
to the globe anterior to the posterior suture if a recession had been
done.4