PREOPERATIVE PREPARATION
The surgeon should exclude patients who are unlikely to tolerate this procedure. A brief discussion with a patient usually reveals those who are unable or unmotivated to cooperate for the postoperative adjustment. Diagnostic tests may be helpful in questionable cases. The ability to tolerate applanation tonometry, forced duction testing, or a cotton applicator applied to the conjunctiva after administering a topical anesthetic have been recommended as methods for assessing a patient's suitability for adjustable suture surgery.8 Before surgery, the patient's anxiety can be relieved and cooperation enhanced by describing the procedure and the adjustment, including the expected level of postoperative discomfort.
ANESTHESIA
Adjustable suture strabismus surgery may be performed using topical, local, or general anesthesia. Topical anesthesia works best with cooperative patients in whom minimal manipulation of the muscle is required. I prefer proparacaine (0.5%) or lidocaine solution (4%), although tetracaine (0.5%) or cocaine (5% to 10%) also are effective. An advantage of topical anesthesia compared with other methods of anesthesia is that a measurement of the ocular alignment and adjustment of the muscle can be performed at the time of the operation.9,10 Local or regional anesthesia in the form of a retrobulbar, peribulbar, or subconjunctival injection of mepivacaine (2%) or lidocaine (2%) is used routinely by some strabismus surgeons in cooperative patients.11,12 After administering local anesthesia, it requires 4 to 6 hours for the extraocular muscles to recover sufficiently to perform an accurate adjustment.13 General anesthesia also is commonly used for strabismus surgery, especially in bilateral procedures and procedures where extensive manipulation of the muscle is necessary. General anesthetics that provide for rapid recovery of consciousness are preferred for adjustable suture strabismus surgery. Intravenous propofol in combination with nitrous oxide has been shown to be an effective general anesthetic agent that allows for faster recovery from strabismus surgery.14,15 Muscle-relaxing agents that act by depolarizing the neuromuscular junction (e.g., succinylcholine) may have a prolonged affect on muscle tone and should be avoided during general anesthesia. Nondepolarizing muscle relaxants do not appear to be a hindrance in adjustable suture strabismus surgery.15 Regardless of whether topical, local, or general anesthesia is used, preoperative analgesics or hypnotics should be avoided, as should all intraoperative or postoperative drugs that might alter the patient's level of consciousness at the time of the adjustment.
The method for preparing the eye and ocular adnexa before surgery is the same as for any strabismus operation. A generous area of the lower lid and lateral canthal skin should also be cleaned with 5% povidone iodine solution. This allows the adjustable sutures to be taped to the skin after surgery.
SURGICAL TECHNIQUE
A variety of adjustable suture techniques have been developed for strabismus surgery. The procedure described here is easy to perform and may be best suited for the surgeon who is not experienced in using adjustable sutures. This technique is similar to nonadjustable suture surgery and requires a minimal amount of manipulation during the adjustment.
A standard limbal conjunctival approach is most commonly used with adjustable suture surgery. Relaxing incisions at the superior and inferior margin of the peritomy provide good access to the muscle. The relaxing incisions should be kept relatively parallel to allow for a conjunctival recession.
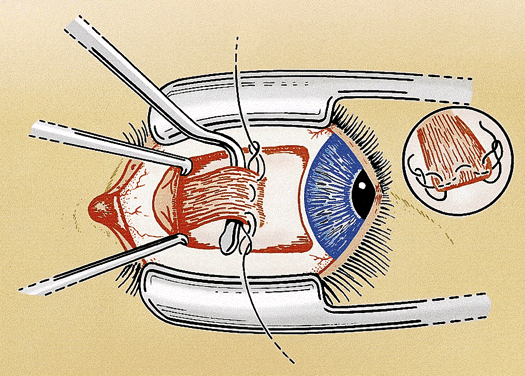
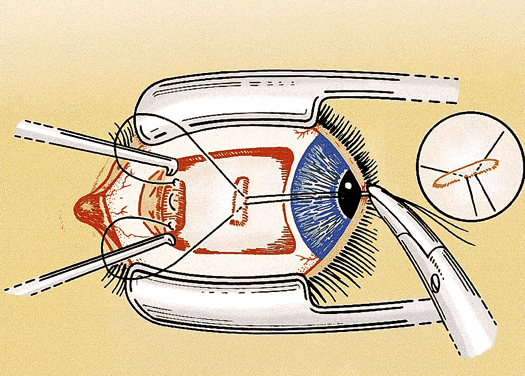
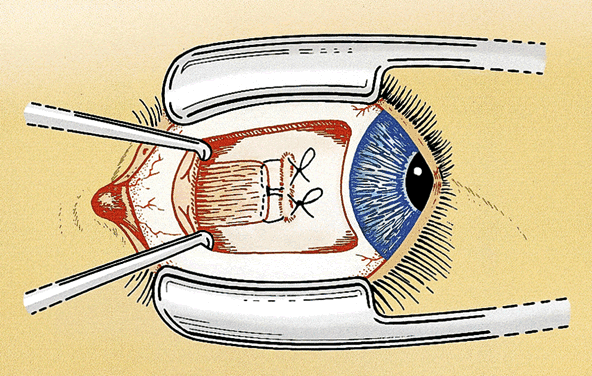
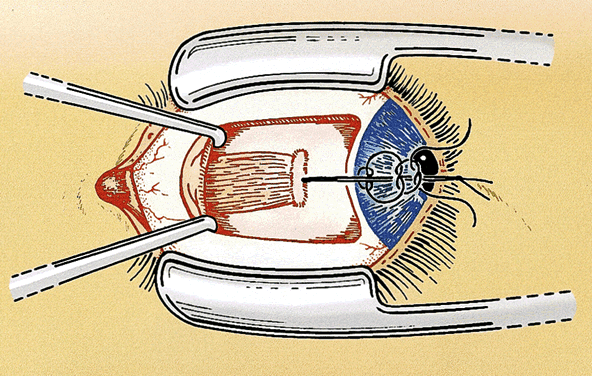
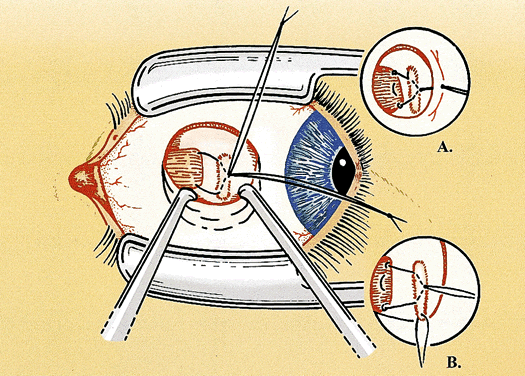
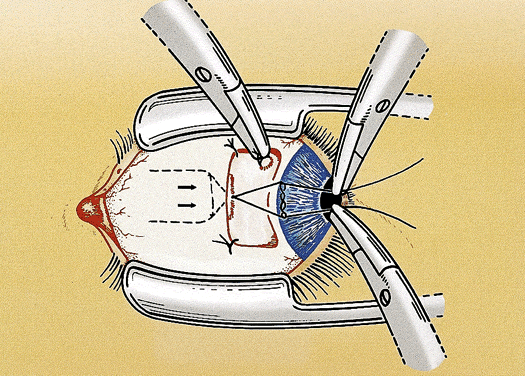
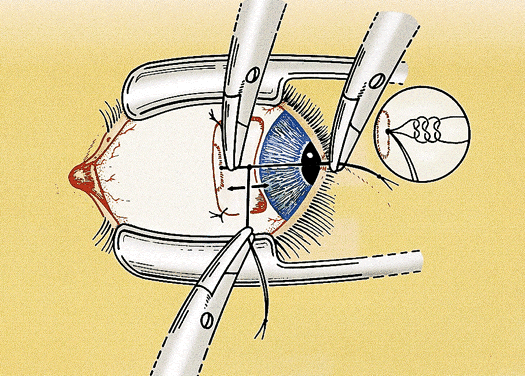
For a rectus muscle recession, the muscle is cleaned of the attachments of anterior tenon's capsule and intermuscular septum in the same manner as for nonadjustable strabismus surgery. The muscle attachments must be cleaned sufficiently to allow for movement during the adjustment. Tissue manipulation is minimized to reduce the postoperative swelling and prevent excessive bleeding, which may hinder the adjustment. A double-armed 6-0 polygalactin suture with spatulated needles (S-24 or TG 100-8) is placed in the muscle tendon 0.5 mm from the insertion with full-thickness lock bites at each edge. Each lock bite incorporates one fourth to one third of the width of the muscle tendon to aid hemostasis and provide a secure muscle attachment during the adjustment (Fig. 1). After the muscle is disinserted, each arm of the suture is passed through a scleral tunnel at the muscle insertion. The tunnels are 4 to 6 mm in length and are placed through half-thickness sclera at a 45° to 60° angle from the insertion. The needles exit the sclera just anterior to the insertion 1 to 2 mm apart (Fig. 2). It is important to carefully clean the episclera and cauterize blood vessels near the scleral tunnels to reduce the chance of suture drag and hemorrhage during the adjustment.
|
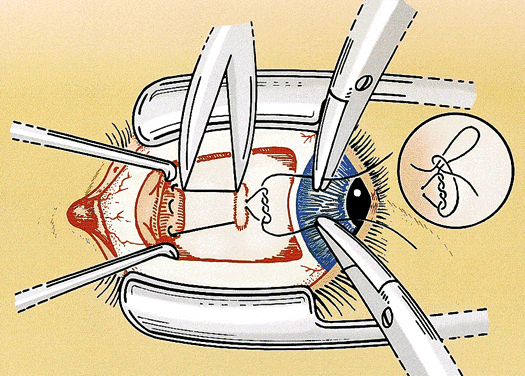
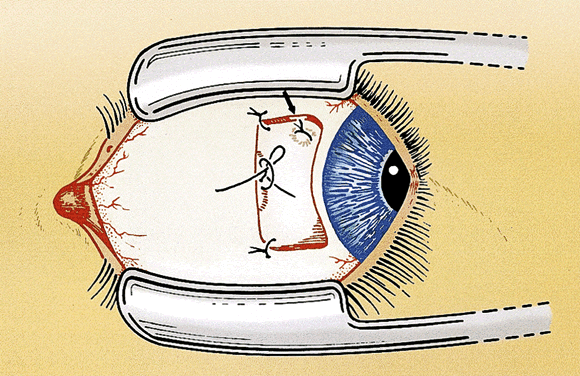
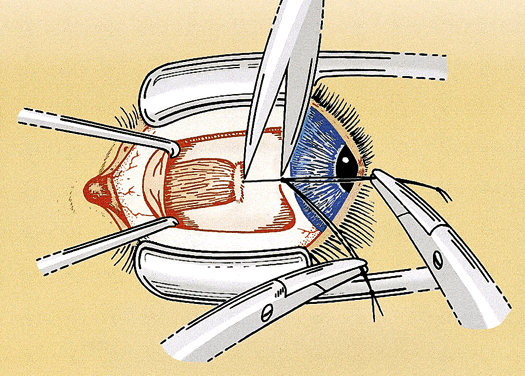
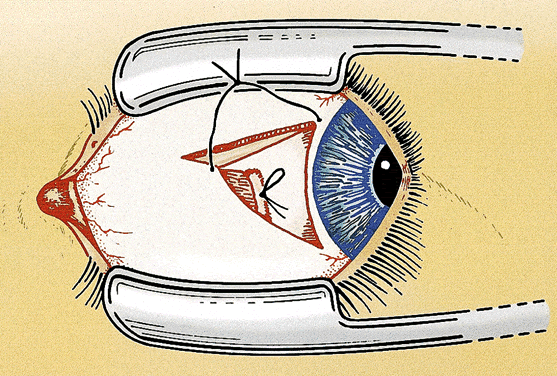
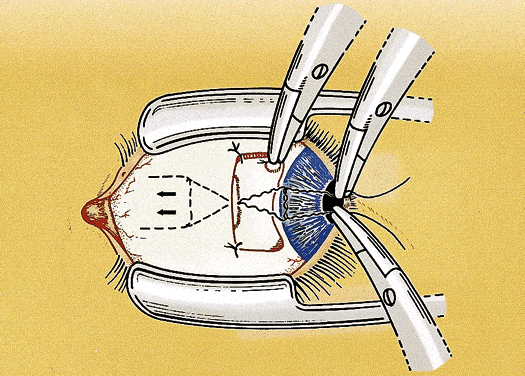
After the needles are removed, the suture ends are tied together loosely with a double throw. The eye is rotated away from the recessed muscle (i.e., laterally if the medial rectus muscle is adjusted) to allow the muscle to retract posteriorly beyond the intended position of recession. A mark is placed on the sclera with Castroviejo calipers preset to the desired amount of the recession from the original muscle insertion. The double throw is tightened until the muscle is pulled up to the scleral mark and the poles of the muscle are equal distance from the insertion. A loop or slip knot is placed over the double throw to secure the suture (Fig. 3). The conjunctiva is closed with 7-0 chromic suture. The conjunctival flap is pulled up until it partially covers the adjustable knot. The relaxing incisions may be closed with additional sutures if necessary (Fig. 4). The ends of the adjustable suture are taped to the skin of the lower lid or tucked into the lower cul-de-sac and held in place with an antibiotic-steroid ointment. An eye patch helps to keep the sutures in place during the immediate postoperative period.
|
|
MODIFICATIONS OF THE ADJUSTABLE TECHNIQUE
Since the introduction of the modern adjustable suture technique, several modifications have been described that offer some advantages. Although usually performed on muscles that are recessed, adjustable sutures also can be used with resected muscles. Most surgeons suggest resecting 1 to 2 mm more than is thought to be required for optimal ocular alignment. This allows for an advancement or recession of the muscle as necessary during the adjustment. For small resections, the single double-armed suture technique used with a muscle recession is acceptable. For larger resections with excessive tension on the muscle, a two-suture technique probably is best (Fig. 5). Both sutures should be adjusted equally if the two-suture technique is used.
Many strabismus surgeons prefer to use a sliding adjustable knot instead of the slip knot. They believe that the sliding knot is easier to adjust, provides a more accurate assessment of the amount of the adjustment, and improves the chances that the suture ends will be pulled up an equal amount. Disadvantages of the sliding knot are that the procedure is more difficult to perform and leaves a bulkier knot, which increases the chances of postoperative irritation.16 The sliding adjustable suture uses the same muscle exposure and suturing methods as previously described. The scleral tunnels also are prepared in the same way as for the adjustable loop suture except that the needles exit the scleral as close to one another as possible. After the sutures have been brought through the tunnels, one suture end approximately 10 cm long is cut off and used to make the sliding knot. The muscle is pulled up and held at the insertion by the sutures. The suture end is tied around both muscle sutures near their exit from the sclera as tightly as possible using three single throws (Fig. 6). One or both ends of the sliding suture are left long for grasping during the adjustment. The sliding suture is moved back and forth on the muscle sutures several times to ensure that it will slide easily during the adjustment. The recession is obtained by pulling the muscle up to the muscle insertion and measuring the desired distance anteriorly from the scleral exit site along the muscle suture. The sliding suture is placed at this position, and the muscle is allowed to retract (Fig. 7). Variations in the conjunctival incision and closure have been described.17,18 Complete closure of a limbal conjunctiva incision can be delayed until after the adjustment. One corner of the conjunctival flap is closed at surgery while the other corner either is left free or loosely attached with a loop of suture. After the adjustment, the loop is cut and the suture ends tied tightly together (Fig. 8). The conjunctival cul-de-sac incision popularized by Parks also can be used during adjustable suture surgery.19,20 An adjustable loop knot or a sliding knot may be used with the cul-de-sac technique (Fig. 9). After the scleral tunnels have been made, one of the needles is removed, and the two suture ends are tied together with a square knot. The conjunctiva and tenon's capsule are repositioned. Using the remaining needle to make a small conjunctival puncture, the square knot is passed through the conjunctiva at a point where it lies directly over the muscle insertion. An adjustable sliding or loop knot is placed over the conjunctiva. The cul-de-sac incision may or may not be closed at the time of surgery, depending on the size of the wound and the surgeon's preference. After the adjustment is completed, the adjustable suture knot is covered with conjunctiva. This is accomplished by lifting the conjunctiva on each side of the small opening created by the sutures and allowing the adjustable suture knot to fall back through the previous puncture site. An alternate method is to adjust the suture directly through the conjunctival cul-de-sac incision. A traction suture is placed near the pole of the muscle insertion to allow for retraction of the conjunctiva.21 After the adjustment is completed, the traction suture is removed and the conjunctiva stroked back into its normal position without suturing.
|
It can be difficult to accurately determine how much the muscle was moved during the adjustment. One approach to this problem is to tie an extra piece of suture around one or both ends of the adjustable suture at a predetermined distance from the scleral tunnels. The sliding adjustable knot works best with this technique. This measuring or marking suture is a reference point for determining the amount of adjustment. The suture is removed after the adjustment is completed.22
Another useful modification of the adjustable suture technique is to use a scleral traction suture. The traction suture reduces the chance of pain and hemorrhage during the adjustment by providing a handle to stabilize the eye. The suture is placed as a moderately deep scleral bite, 2 to 4 mm from the limbus, and tied in a loose loop. It is best to place the traction suture inferior and anterior to the muscle insertion for horizontal muscles and temporal and anterior to the muscle insertion for vertical muscles (see Fig. 4). The ideal suture for adjustable strabismus surgery is absorbable and strong, ties securely, and offers minimal tissue resistance.23 Most strabismus surgeons use 6-0 synthetic absorbable suture made of polyglactin 910 or polyglycolic acid. Either suture can be used for all of the adjustable techniques and modifications. Spatulated needles are preferred by most surgeons for adjustable suture surgery. The conjunctiva also can be closed with the same suture but a more rapidly absorbing suture (i.e., 6-0 or 7-0 plain gut or chromic gut) is tolerated better by most patients.
Adjustable suture strabismus surgery is almost exclusively restricted to rectus muscles. Suture adjustment is difficult on the oblique muscles because of the posterior orientation of the muscle insertion. A technique for tucking the superior oblique tendon that provides a limited postoperative adjustment has been described.24 An adjustable suture approach to the anterior fibers of the superior oblique tendon for the treatment of excyclotorsion also has been developed.25