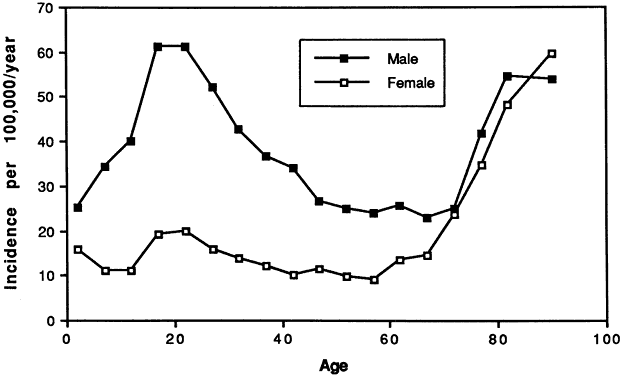
TABLE 56-1. Incidence of Ocular Trauma
| Location Setting | Population Studied | Type of Data | Case Definition of Ocular Trauma | Annual Incidence Rate per 100,000 Population |
| Alabama(1982-86)9 | All ages | Prospective trauma registry | Severe injury | 7.7 |
| Maryland (1979-86)10 | All ages | Hospital discharge data analysis | Principal hospital discharge diagnosis (principal and secondary discharge diagnoses) | 13.2 (27.3) |
| United States(1984-86)11 | All ages | Hospital discharge dataanalysis | Principal hospital discharge diagnosis (principal and secondary discharge diagnoses) | 13.2 (29.1) |
| Stockholm, Sweden(1974-79)20 | All ages | Retrospective studyusing hospitalization case records | Injury requiring hospitalization | 6.1 |
| Scotland (1991-92)21 | All ages | Prospective study on all eye trauma hospitalizations | Injury requiring hospitalization | 8.1 |
| Victoria, Australia(1989-91)22 | All ages | Prospective study onall eye trauma hospitalizations | Injury requiring hospitalization | 15.2 |
| Papua New Guinea(1984-95)28 | All ages | Retrospective study onall eye clinic visits related to trauma | Medically treated injury | 39 |
| Wisconsin(1978-79)13 | All ages | Prospective study on eyecasually room visits | Medically treated injury (injuryrequiring hospitalization) | 420 (47) |
| Newcastle, England(1992)24 | All ages | Prospective study on eye casually room visits | Medically treated injury (injuryrequiring hospitalization | 720 |
| Baltimore (1985-88)17 | 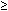 40 yr 40 yr | Population-based interview | Any injury (medically treated injury) | 490 (400) |
| New England (1985)16 | 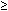 18 yr 18 yr | Population-based interview | Medically treated injury | 980 |
| California (1988)12 | All employed persons | Hospital discharge data and workers compensation claims analysis | Principal hospital discharge diagnosis plus workers compensation as the principal source of payment (principal and secondary discharge diagnoses) | 1.8 (3.0) |
| Maryland (1982)62 | 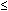 16 yr 16 yr | Hospital discharge data analysis | Principal hospital discharge diagnosis | 15.2 |
Eye injury registries can be an important and useful source of information if they are linked to a population perspective. The National Eye Trauma System (NETS) registry collected data on open globe injuries in 48 collaborating centers in 28 states7 and provided basic demographic, clinical, and etiologic information on these severe injuries. However, participation in the NETS is voluntary, only penetrating injuries are reported, and estimates of population burden are not available because ascertainment of these injuries is not complete for a defined population. Similarly, the Eye Injury Registry of Alabama collects information only on severe eye injuries and is not compulsory.8,9 Morris's study reported an annual incidence of severe ocular trauma with significant anatomical or structural damage of 7.7 per 100,000.9 In comparison, a Swedish study estimated an annual incidence of 6.1 per 100,000 for open globe injuries.20
Hospital discharge data are another source of information on ocular injury and can provide good estimates of ocular injury incidence.10–12 In both Maryland and the United States as a whole, using a definition of a principal hospital discharge diagnosis of ocular injury, the annual incidence was estimated to be 13.2 per 100,000. If secondary discharge diagnoses of ocular trauma were included, the incidence was between 27.3 and 29.1 per 100,000 per year. Hospital discharge data have shown a decline in admission for ocular trauma over time, with a 25% decline in incidence of hospitalization for ocular trauma from 1979 to 1986. This appears to be related to changing indications for hospitalization, especially for traumatic hyphema.10 Even in the United States, there is significant regional variation in the incidence of hospitalization for ocular trauma. For example, the New England and Pacific regions were found to have age- and gender-adjusted rates 25% or more below the national average, but the West North Central region had a rate 40% above the average.11 Comparable data are available from other countries. A prospective study on all patients admitted to Scottish hospitals for ocular trauma indicated an annual incidence of 8.1 per 100,000 individuals.21 A study in Victoria, Australia estimates an annual incidence of eye injuries requiring hospitalization of 15.2 per 100,000.22 Different standards of clinical practice among countries and hospitals likely affect the rate of hospitalization as well as other factors, such as age and socioeconomic distributions.
Data at eye emergency departments in hospitals capture eye injuries that usually need immediate medical attention. Because a large number of such cases are relatively minor injuries that do not require hospital admission, they provide a broader perspective on the problem at the population level than do hospital discharge data. An important prerequisite in estimating incidence using data from eye emergency departments is a well-defined population served by a single hospital or a few hospitals, and reasonable justification that the population will not seek treatment elsewhere. Karlson and Klein reported on patients with ocular trauma, seen in emergency rooms or in hospitals, among residents of Dane County, Wisconsin, and estimated an incidence of 420 per 100,000 per year, of which only 11% were admitted to a hospital.13 These data suggested an incidence of hospitalization of 47 per 100,000, about four times higher than in either Klopfer's or Tielsch's study. However, the total number of hospitalizations was extremely small and a direct comparison is difficult to make because ocular injury was not the usual reason for hospitalization. At the University Hospital of Umea in Sweden, 927 eye injuries were treated during a one year period, an estimated annual incidence of 810 per 100,000 population.23 A prospective study on all patients presenting to eye casualty services in Newcastle, England showed an annual incidence of 720 per 100,00024; caution should be exercised in interpreting this figure, however, because the study was conducted during a period of 8 weeks. Although incidence rates cannot be calculated from most other studies because of a lack of a well-defined denominator, they provide valuable information on the etiology, severity, and consequences of ocular injury.14,15,25
Population-based studies provide data on injuries not requiring medical attention at emergency rooms or admission to hospitals and better reflect the burden of this problem in the population. Two such studies have used questionnaires to estimate the incidence of ocular injuries.16,17 Glynn and colleagues surveyed a randomly selected New England population 18 years of age or older and found an annual incidence of 980 ocular injuries per 100,000 individuals.16 This suggested that more than 90,000 eye injuries require medical attention annually in New England alone. Katz and Tielsch estimated a rate of 400 per 100,000 in a population 40 years of age or older from the Baltimore Eye Survey.17 This was similar to an incidence of 300 per 100,000 in Glynn's study for individuals more than 40 years of age.16 An additive risk of ocular trauma occurred with age; the cumulative lifetime prevalence of ocular injury was nearly 15%.17
Limited information is available regarding the incidence of ocular trauma in developing countries. Blindness prevalence studies have indicated that ocular trauma does not appear to be a major problem26,27; however, such surveys usually contain detailed examinations for only those subjects who have bilateral vision loss, thus excluding most ocular injuries, which are unilateral. A recent retrospective chart review of all ocular trauma cases seen in Papua New Guinea estimated an incidence of 39.1 per 100,000.28 A survey of patients admitted to a hospital for ocular trauma in Malawi, in south-east Africa, showed that eye trauma was relatively common, occurring most frequently in children, young adults, and males.29 Most of the injuries occurred under domestic circumstances and were associated with chopping and gathering wood.
BLINDNESS AND OTHER CONSEQUENCES FROM OCULAR TRAUMA
The ocular morbidity and burden of ocular trauma are enormous. As noted earlier, bilateral blindness rates do not provide an accurate population-based perspective of the burden of ocular trauma because of the unilateral nature of the disease. Sommer and coworkers found in the Baltimore Eye Survey that the prevalence of bilateral blindness caused by ocular trauma was 75 per 100,000 and that eye injuries accounted for only 5.6% of blind eyes among all bilaterally blind persons.18 Although the study found no case of bilateral blindness caused by ocular trauma in whites, 9.5% of blind eyes among bilaterally blind black persons were from trauma. Another source of data is the Model Reporting Area Study (MRA), which collected information from 16 states in the United States that agreed to a common format and definition for reporting blindness registration. Injury or poisoning accounted for 3.6% of all incident cases of blindness, with an annual incidence of blindness registration from ocular injury of 0.48 per 100,000 in 1970.19 This was significantly lower than rates estimated in the Baltimore Eye Survey,18 in part because of the incomplete ascertainment of blind persons in the MRA system. In other countries, the rate of bilateral blindness from ocular trauma is also small. In a Scottish study, no patient was registered blind on discharge from the hospital during the one year study period.21 The Israeli Ocular Injuries Study found that bilateral blindness occurred in only six out of 2,276 patients (260 per 100,000) hospitalized for ocular injuries.30 In Sweden, an annual incidence of 6.1 per 100,000 for potentially blinding open globe injuries was reported.20 Limited information is available about actual rates of ocular injury in developing countries but blindness prevalence surveys indicate that the absolute rates of blindness from trauma appear to be small. In Nepal, 860 per 100,000 people had either a history or clinical signs of trauma, but less than 40% had any visual impairment.31 Only 2.4% of cases of bilateral blindness, or an absolute prevalence of 20 per 100,000, were due to trauma; this rate is approximately three times lower than the prevalence found in the Baltimore Eye Survey.18 Population-based studies conducted in Africa failed to find any cases of bilateral blindness caused by trauma.26,32 Although accurate estimates of the prevalence or incidence of blindness from ocular trauma in most populations are still not available, it would appear that ocular injuries play a relatively minor role in the etiology of bilateral blindness.
Although ocular trauma accounts for only a small proportion of cases of bilateral blindness, it is an important cause of monocular blindness. In rural Kentucky, trauma accounted for 40% of monocular blindness, or a population prevalence of 13.2 per 1000.3 In east Baltimore, the prevalence of trauma-associated monocular blindness was 6.6 per 100017 and in Nepal, 2.4 per 1000.31 Of patients admitted to a hospital for ocular trauma in the Scottish study, 10.7% were unilaterally blind at discharge.21,33 Because blinding ocular injuries are often associated with multiple organ injuries with high case fatality, cross-sectional surveys underestimate the magnitude of this problem.
From a public health perspective, neither bilateral or unilateral blindness rates provide a complete context of ocular trauma for society. Another important viewpoint is reflected in the economic costs associated with ocular injury. Severe ocular trauma requires expensive hospitalization and specialist treatment, and often prolonged follow-up and visual rehabilitation. An overall picture of the economic burden requires an estimation of both direct costs of treating ocular injuries and indirect costs resulting from the injuries (such as time lost from work and family caregiving).
Direct costs of ocular trauma have been investigated by Tielsch and Parver. They estimated that more than 227,000 hospital days and approximately 200 million dollars in hospital charges may be directly related to hospitalization for ocular injuries each year, based on Maryland hospital discharge data.34 Even these figures on direct costs may be considered an underestimation because physician fees, investigation charges, follow-up charges in the outpatient setting, and medications were not included in these totals. In addition, Veterans Administration hospital admissions were not included in the calculations in this study.
The indirect, secondary economic impact of ocular trauma is harder to estimate. Work-related ocular injuries usually affect young adults who are in their most productive years. Three quarters of work-related open globe injuries reported in the NETS study occurred in individuals less than 40 years of age.7 Schein and colleagues observed that patients with open globe injuries had an average of 70 days of medical leave from work and that 40% of those with open globe injuries sustained at work were pursuing costly legal action against their employers.15 Munoz estimates that in the United States, around 5 million dollars is spent on ocular trauma in direct and indirect costs per urban trauma center.5 Similar economic burdens can be expected in other developed countries. Fong estimated that 155 million dollars a year may be spent on hospitalization for the estimated 116,000 annual cases of ocular injury in Australia.22 The full socioeconomic impact of ocular injuries must be studied further to provide a more complete picture of the public health significance of ocular trauma.