PHYSICAL DEFINITION OF UVR
The spectrum of nonionizing radiation ranges from short-wavelength UVR (wavelength 100 nm) to far-infrared radiation (1 mm or 100,000 nm) (Fig. 1). The visible spectrum lies between 400 nm (indigo) to 760 nm (red). Beyond the visible spectrum is infrared radiation, and below the visible spectrum are the shorter wavelengths of nonionizing radiation called ultraviolet radiation (UVR). Although UVR is only 5% of the sun's energy, it is the most hazardous portion encountered by humans. The physical spectrum of UVR ranges from 100 to 400 nm. However, much of the nonionizing radiation is absorbed by the earth's atmosphere. Wavelengths less than 290 nm are totally absorbed by the ozone layer in the stratosphere, and longer wavelengths are absorbed to a lesser extent. Thus, in nature, UVR less than 290 nm does not reach the earth's surface and is not encountered.6
Based on the biologic effects of the different wavelengths or bands, UVR has been subdivided into three bands: UV-A (400 to 320 nm), UV-B (320 to 290 nm), and UV-C (290 to 100 nm).7 UV-A, or near UVR, produces tanning (the browning of the skin due to an increase in the skin content of melanin) and photosensitivity reactions. UV-A is emitted by so-called black lights, which are often used to make objects fluoresce and are also used in tanning salons. UV-B causes sunburn (painful erythema and blistering), and increased exposure to UV-B is associated with an increased rate of skin cancer.6–9 UV-C, which is germicidal and may also cause skin cancer, is not normally encountered on the earth's surface and comes entirely from artificial sources such as germicidal ultraviolet lamps or arc welding.
ENVIRONMENTAL, TEMPORAL, AND GEOGRAPHIC VARIATIONS IN ULTRAVIOLET RADIATION
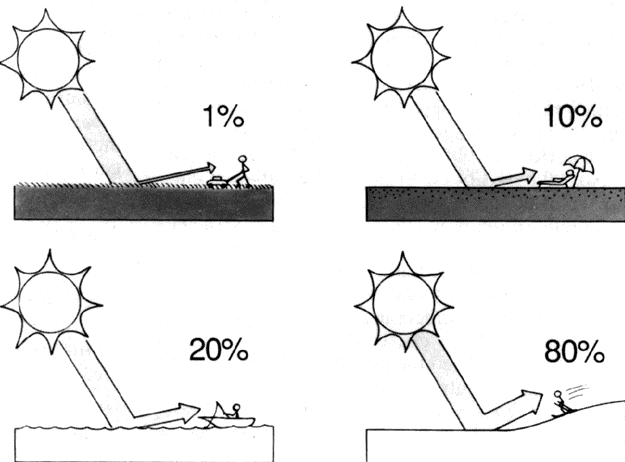
UVR is scattered across the whole sky by the Rayleigh effect, just as blue light is scattered.8 Light or broken clouds do not significantly reduce the level of UVR, although levels are reduced by heavy cloud cover.8 A sky with a clear horizon for 360° provides for maximal exposure; when hills, trees, or buildings obstruct part or all of the horizon, the UVR exposure is reduced proportionally.10 UVR can also be reflected by the ground, the amount dependent greatly on the type of surface (Fig. 2). Grass and soil reflect only 1% to 5% of UV-B, water 3% to 13%, sand and concrete about 7% to 18%, and fresh snow up to 88%.10
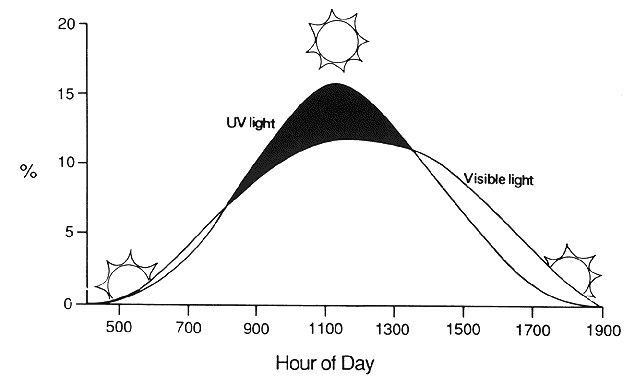
As the sun makes its daily transit, the spectral content of sunlight changes substantially (Fig. 3). At low incident angles, nearly all visible and ultraviolet energy is reflected or absorbed by the atmosphere, giving the familiar reddish hue to early morning and late evening sunlight. The UV-A and UV-B content of sunlight increases as the sun reaches its zenith and progressively decreases during the afternoon. Similarly, the farther from the equator, the more oblique is the angle of sunlight incidence and the lower the UVR level on the ground. Many people have learned the hard way that an hour's exposure to tropical sunlight imparts a far greater dose of UV-B than does an hour on the beach in New England or the Pacific Northwest. As the Earth tilts to produce changing seasons, so too does the angle of sunlight incidence and the resulting UVR content of sunlight, with summer sunlight imparting far greater doses of UV-B than sunlight of other seasons.
The ambient dose of UVR also increases somewhat at higher altitudes, because there is less atmosphere to filter the sun's energy. UV-B exposure increases approximately 20% per 10,000 feet. Climbers have frequently discovered that they are vulnerable to sunburn even when the sun seems to exert little warming effect. Persons climbing and skiing on snow-covered peaks are at particular risk because of the extremely high ultraviolet reflectivity of snow and ice.
The eyes are normally protected and shielded from UVR by a number of factors11,12aand only receive a small fraction of ambient UV-B under normal circumstances. The normal horizontal alignment of the eyes and the orbits significantly reduces ocular exposure to whole-sky irradiation. Further anatomical protection is provided by the brows, the nose, and the cheeks.13 The eyelids provide protection that is further enhanced by squinting, a common reflex in bright sunlight. The eyes are relatively unprotected laterally, although the transmission of UVR by internal reflection in the cornea may lead to a concentration of ultraviolet irradiation at the nasal limbus.14 Other personal factors that can decrease ocular UVR exposure in a given environment include wearing a hat and protective eyeglasses.11,12 Taken together, these different factors result in an ocular exposure that is between 7% and 17% less than the ambient UVR level.12
OCULAR TRANSMISSION OF ULTRAVIOLET RADIATION
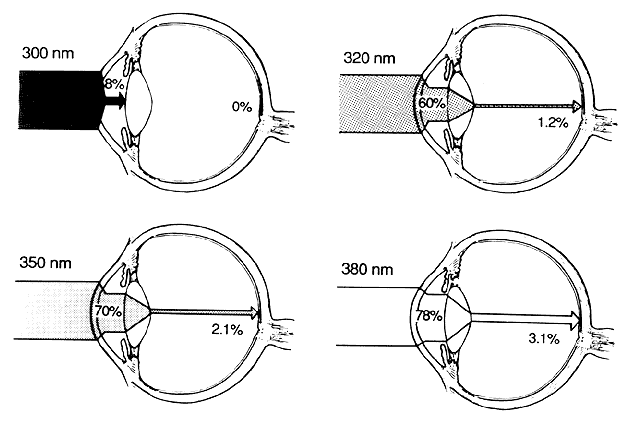
Only a fraction of the UVR entering the eyes reaches the retina-a fact with important photobiologic implications (Fig. 4). The amount of radiation that is absorbed determines the potential for damage to the absorbing tissue. Energy from the dissipation of the absorbed radiation results in tissue damage. Radiation that is not absorbed by a superficial tissue will be transmitted and can affect deeper tissues.
The cornea absorbs almost 100% of UV-C radiation (below 290 nm), but transmission rapidly increases for longer wavelengths, so that, for instance, 60% of radiation at 320 nm is transmitted by the cornea.15–18 A normal young human lens absorbs most UVR below 370 nm. As the human lens yellows with age, it absorbs even more UV-A and also shorter blue wavelengths.18,19 In adults, less than 1% of radiation between 320 and 340 nm and only 2% of radiation of 360 nm reaches the retina.20 The lens is exposed to and absorbs most of the UV-B entering the eye.
MECHANISMS OF PHOTOTOXICITY
The energy carried by a photon is directly proportional to its frequency; thus, the shorter the wavelength, the higher the energy. A photon's energy is absorbed by the atom or molecule with which it collides. Low-energy infrared photons carry enough energy to affect the rotational or vibrational state of an atom or a molecule and produce warming. Higher-energy UVR photons can alter the energy state of the electrons, making the atom or molecule relatively unstable, leading to oxidative reactions including cross-linking and denaturation of proteins and free-radical formation. Higher-energy photons such as gamma rays cause an electron to be removed entirely from the molecule, thereby causing ionization.
The capacity of a given atom or molecule to absorb radiant energy is dependent on its physicochemical properties, and the characteristics of a tissue are in turn dependent on the properties of its constituents. The lens proteins are rich in the amino acid residues of tryptophan, tyrosine, and phenylalanine, which absorb most of the radiant energy below 300 nm. Cross-linking of these proteins is implicated in the pathogenesis of cataract. Other chromophores and pigments in the lens appear to absorb most of the energy in the 300 to 400 nm range.21