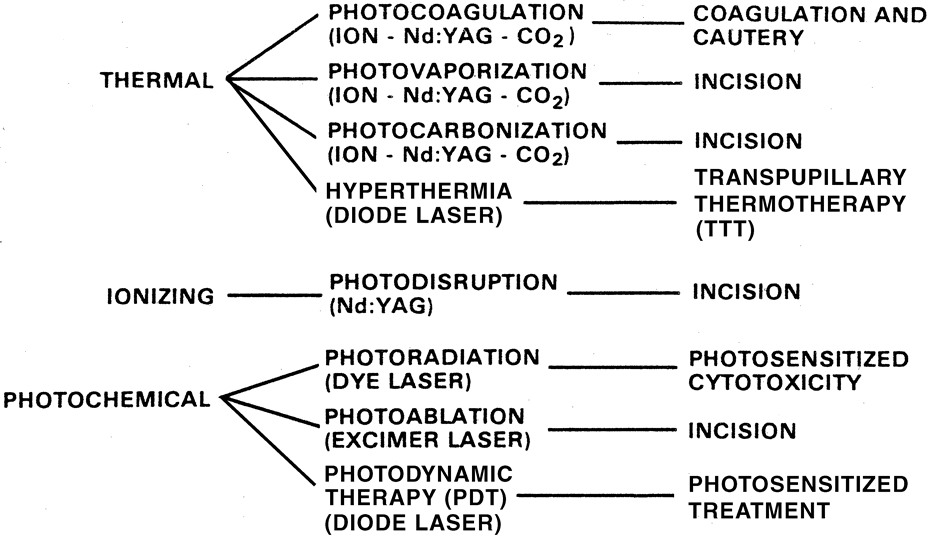
Optical characteristics of ocular tissues play an important role in the
effectiveness of photocoagulation in the retina. Laser light traveling
through the eye toward the target tissue is affected by the degree of
reflection, scattering, and absorption of laser energy by ocular tissues
and by media opacities. Other important factors affecting laser photocoagulation
are the degree of absorption by ocular pigments, specific
wavelengths used, spot size, power applied, and the exposure time
used to produce the desired reaction in the retina (Fig. 2).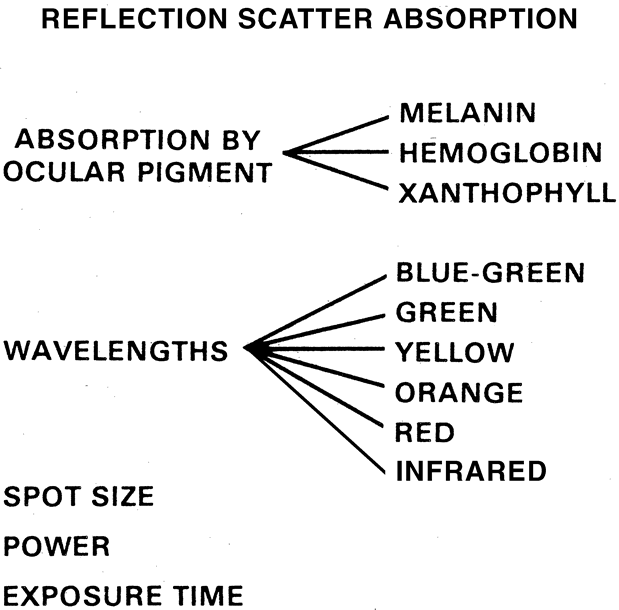 Fig. 2. Factors in retinal photocoagulation. Fig. 2. Factors in retinal photocoagulation.
|
REFLECTION, SCATTERING, AND MEDIA ABSORPTION When a laser beam irradiates a biological tissue, this optical radiation
usually undergoes a series of processes, which can ultimately affect
the power of the laser beam at the target tissue. Reflection of the beam usually occurs when an abrupt change in refractive
index occurs, most commonly at the interface of different refractive
media. The reflection of the beam depends on the texture of the reflective
surface: the smoother the surface, the cleaner the reflection. The
amount of reflection is usually not a major issue aside from its ability
to decrease the useful power density of the laser. Scattered light represents the loss of laser energy available to reach
the target tissue. This loss is due to absorption by ocular tissues other
than the target tissue and by reflection away from the target or back
out of the eye. Increased scattering occurs with shorter wavelengths. The
short blue wavelength scatters more than the longer red light, which
explains why lesions produced in the retina with argon blue-green
light are larger than those produced with the red wavelength
using the same size spot at the corneal level. Importantly, media opacities
also increase scattering and decrease the energy available to produce
the retinal lesion. The power density needed to penetrate a media
opacity to produce a satisfactory retinal lesion suddenly becomes too
great when applied to another area through clear media, resulting in
a severe reaction. Starting in early adulthood and advancing with age, scattering in the ocular
media increases, more with the shorter blue wavelength than with
the green light and longer wavelengths. For example, three times more
power is needed at the cornea when using blue light than green, and approximately
two times more power is needed with green light than with
the yellow to produce the same retinal lesion. The presence of yellow pigment in the aging lens produces increased scattering
and absorption at the level of the lens, most noticeably with
the short blue wavelength. Scattering and absorption at the level of the
lens may increase temperature, resulting in damage to the lens fibers
and decreased energy reaching the retina. The difference between scattering
and absorption is that scattering processes do not really alter
the energy balance, while absorption transfers energy from radiation
to matter. Absorption by ocular pigments has a great deal to do with
the power density at which a laser beam affects a target tissue. ABSORPTION BY OCULAR PIGMENTS Laser light is mainly absorbed in ocular tissue by three pigments: hemoglobin, melanin, and
xanthophyll. The reaction of retinal tissue to the
irradiation with a given wavelength, time setting, and power density
varies depending on the concentration of these three pigments (Fig. 3). Melanin strongly absorbs all ultraviolet and invisible wavelengths. However, this
absorption by melanin decreases with increasing wavelengths. Hemoglobin
has strong absorption in the violet (420 nm) and
green (514 nm) wavelength. Deoxygenated hemoglobin
absorbs red more strongly than does oxyhemoglobin. Xanthophyll, which
is the pigment most densely distributed in the macular area, absorbs
the blue wavelength (460 nm). 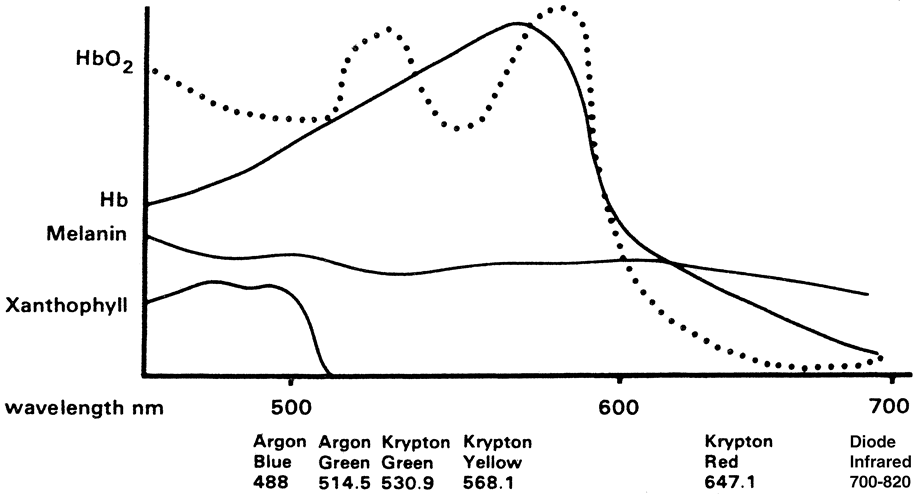 Fig. 3. Absorption coefficients of ocular pigments in relation to wavelengths. Fig. 3. Absorption coefficients of ocular pigments in relation to wavelengths.
|
WAVELENGTHS Several wavelengths are clinically available for photocoagulation (see Fig. 2). The argon laser with blue and green wavelengths was the laser used
for many years in the treatment of choroidal retinal diseases. The
majority of commercial argon lasers in the past used a light beam that
was 70% blue (488 nm) and 30% green (514.5 nm). Blue
light, however, has many disadvantages (Fig. 4). It is scattered more in the media than is green, yellow, or red, and
the scattering increases with aging of the ocular media. Higher
levels of energy at the corneal level are needed to obtain an appropriate
retinal burn compared with longer wavelengths, especially in older
persons. 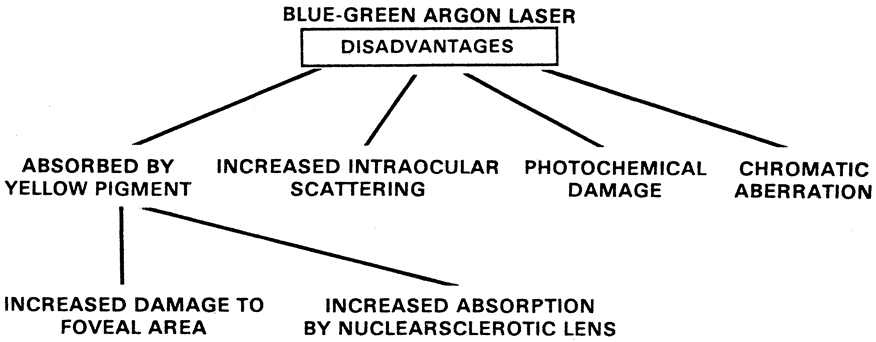 Fig. 4. Disadvantages of the blue-green argon wavelength. Fig. 4. Disadvantages of the blue-green argon wavelength.
|
Photochemical damage is higher for shorter wavelengths than for longer
wavelengths, and scattered light could possibly produce damage in the
retina adjacent to the area treated. This is most important when large
amounts of irradiation are applied in the retina (such as in panretinal
photocoagulation in the treatment of diabetic retinopathy). Most importantly, blue light is absorbed by the xantbthophyll (yellow) pigment
present in the inner and outer plexiform layer of the
macular area, producing increased damage during photocoagulation of
this area. This increases the risk of central scotomas following treatment
with blue laser light. Figure 5 shows marked destruction of the inner layers of the retina in experimental
studies when blue light is used for photocoagulation.7,8 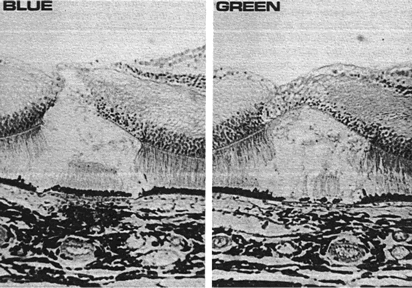 Fig. 5. Histologic sections of the foveas of macaque monkeys. With blue light, all
retinal layers are destroyed by coagulation; with green light, the
inner layers are preserved and the outer layers are destroyed. (Pomerantzeff
O, Kaneko H, Donovan R et al: Effect of the ocular media
on the main wavelengths of argon laser emission. Invest Opthalmol Vis
Sci 15:70, 1976.) Fig. 5. Histologic sections of the foveas of macaque monkeys. With blue light, all
retinal layers are destroyed by coagulation; with green light, the
inner layers are preserved and the outer layers are destroyed. (Pomerantzeff
O, Kaneko H, Donovan R et al: Effect of the ocular media
on the main wavelengths of argon laser emission. Invest Opthalmol Vis
Sci 15:70, 1976.)
|
The use of the blue wavelength has been discontinued for use in photocoagulation
because of its destructive properties and in favor of other
wavelengths, most commonly the green wavelength. The green argon laser
light has a wavelength of 514 nm. It is the most widely available and
popular laser light for retinal photocoagulation and can be found in
lasers made entirely for pure green output and blue-green lasers
with filters providing the pure green wavelength. Green and yellow wavelengths have similar advantages (Figs. 6 and 7). Both wavelengths are absorbed by hemoglobin in blood vessels and
are not absorbed by the xanthophyll pigment of the macular area. However, yellow
is at least two times better absorbed by hemoglobin and is
a more effective wavelength in the destruction of abnormal vascular
structures of the eye.9 Much less energy is necessary to produce a retinal lesion with the yellow
wavelength than with the green, and, as shown in animal experiments, less
involvement of the inner layer of the retina is observed with
either wavelength as compared with the blue (Fig. 8; see Fig. 5). 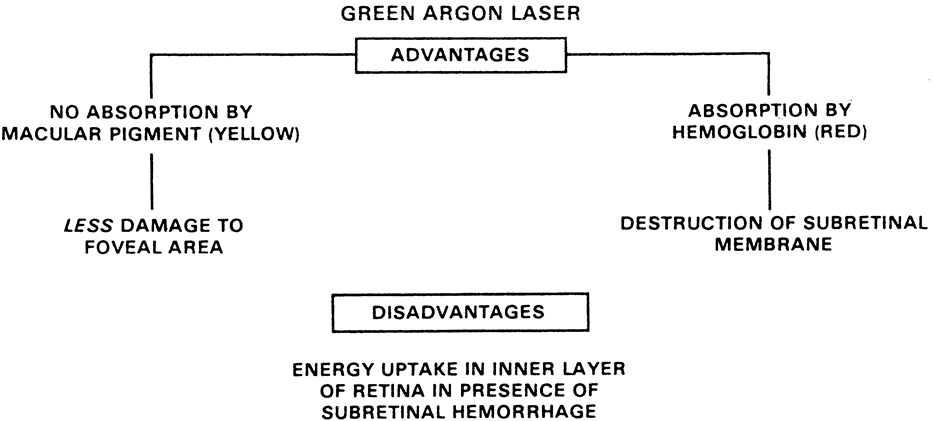 Fig. 6. Advantages and disadvantages of the green argon wavelength. Fig. 6. Advantages and disadvantages of the green argon wavelength.
|
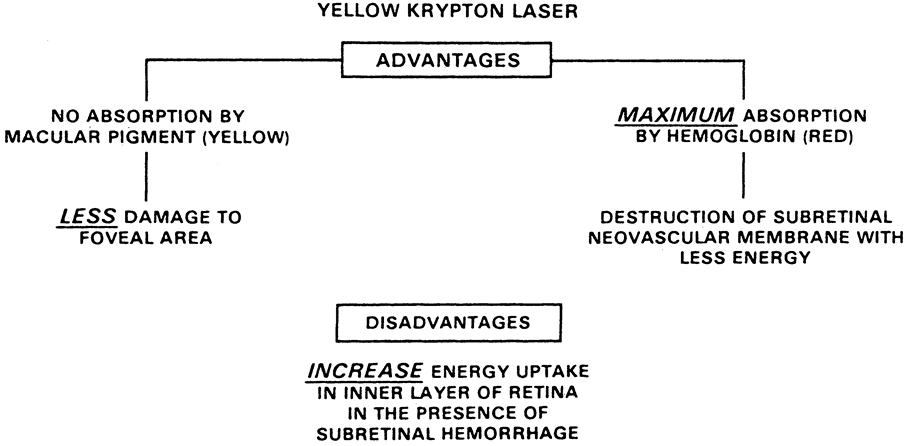 Fig. 7. Advantages and disadvantages of the yellow krypton wavelength. Fig. 7. Advantages and disadvantages of the yellow krypton wavelength.
|
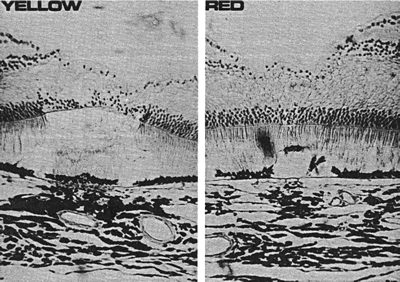 Fig. 8. Histologic sections of the foveas of macaque monkeys. With krypton yellow, the
lesion is similar to that produced with argon green. With krypton
red, the damage is limited to the level of pigment epithelium. (Pomerantzeff
O, Kaneko H, Donovan R et al: Effect of the ocular media
on the main wavelengths of argon laser emission. Invest Ophthalmol
Vis Sci 15:70, 1976.) Fig. 8. Histologic sections of the foveas of macaque monkeys. With krypton yellow, the
lesion is similar to that produced with argon green. With krypton
red, the damage is limited to the level of pigment epithelium. (Pomerantzeff
O, Kaneko H, Donovan R et al: Effect of the ocular media
on the main wavelengths of argon laser emission. Invest Ophthalmol
Vis Sci 15:70, 1976.)
|
Green and yellow have some disadvantages, namely, absorption occurs at
the vitreous level in cases of vitreous hemorrhage, resulting in possible
tissue damage and a decrease in energy available to produce the desired
lesion. Furthermore, if a layer of blood is present in the inner
layer of the retina, increased energy uptake is produced in the inner
layer of the retina, preventing treatment of deeper structures, such
as a subretinal neovascular membrane (Fig. 9). The yellow laser wavelength is not frequently used because of the
cost of instrumentation and equipment. It still remains, however, the
best wavelength to treat vascular lesions because of the increased
absorption by oxyhemoglobin, which reduces the amount of power required
to obtain the tissue reaction needed to coagulate the vascularized tissue. |
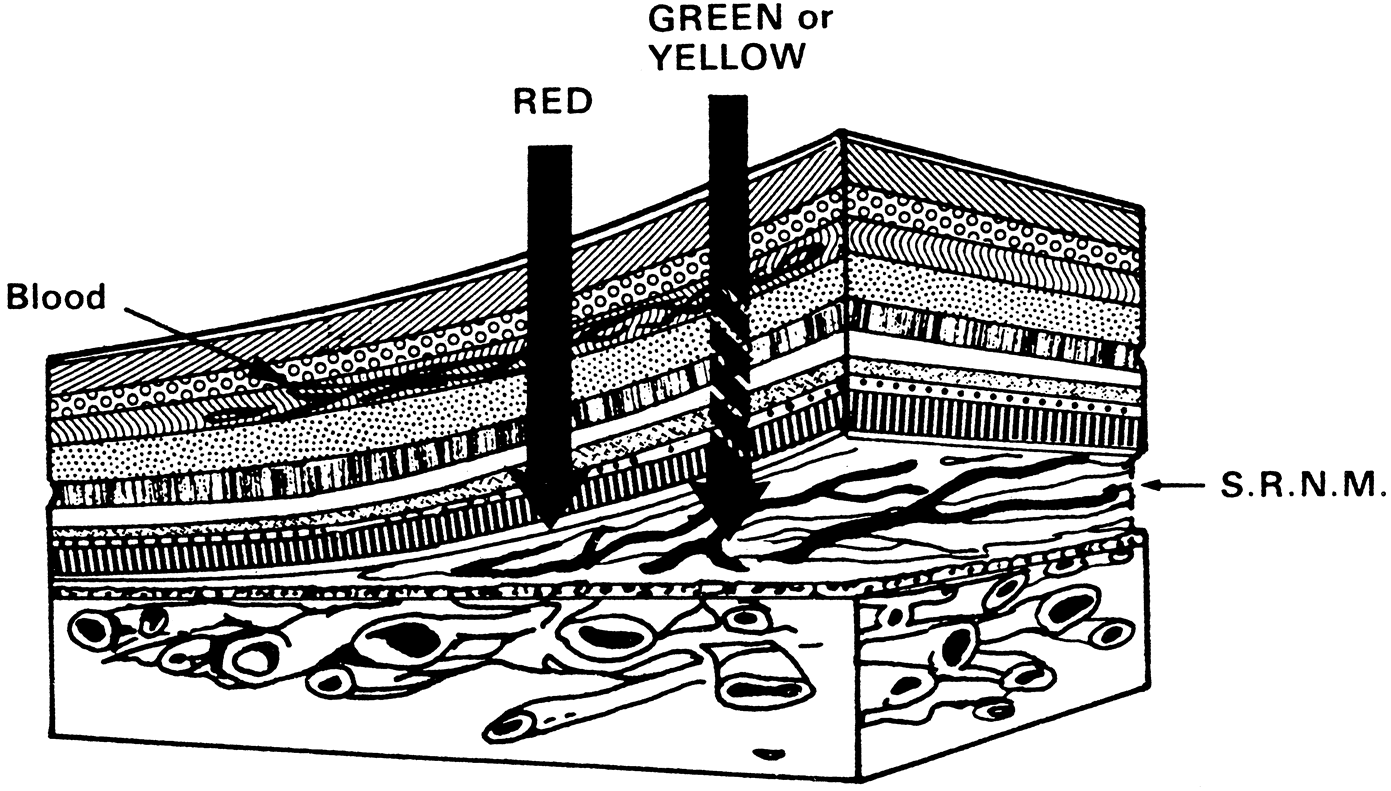 Fig. 9. There is increased energy absorption in the inner layer of the retina in
the presence of blood with green and yellow wavelengths and decreased
uptake with red krypton while treating the deeper subretinal neovascular
membrane (S.R.N.M.).
Fig. 9. There is increased energy absorption in the inner layer of the retina in
the presence of blood with green and yellow wavelengths and decreased
uptake with red krypton while treating the deeper subretinal neovascular
membrane (S.R.N.M.).
|
The red wavelength has been used in some retinal diseases, such as age-related
macular degeneration. The red wavelength, such as that
produced by red krypton, is very useful and has unique features (Fig. 10). It penetrates more deeply through ocular structures, producing
its absorption in the melanin at the deeper retinal layer close to the
choroidal vessels, the most likely source of the abnormal subretinal
neovascular membrane in age-related macular degeneration. 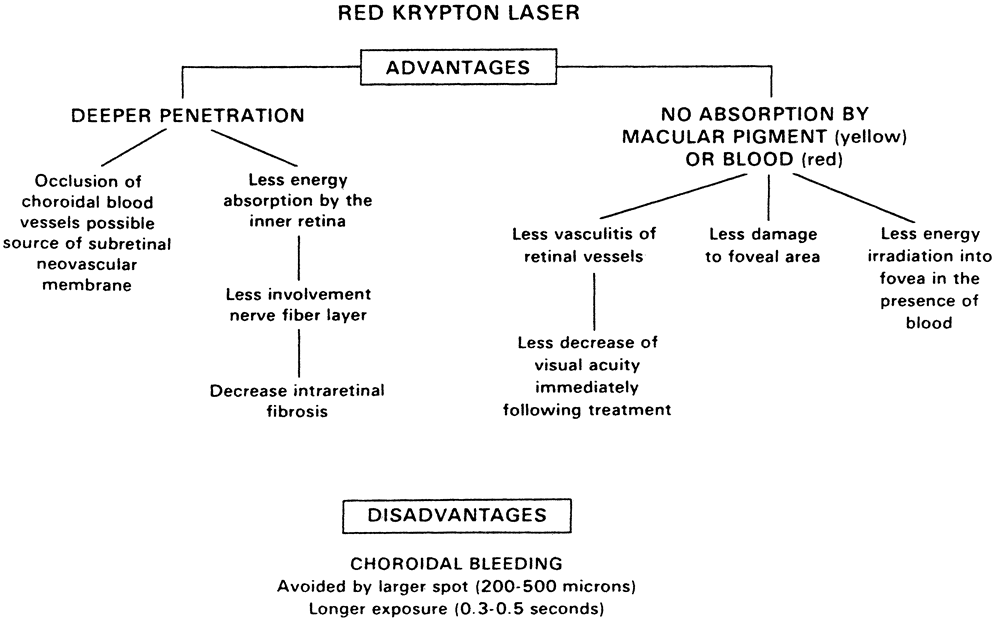 Fig. 10. Advantages and disadvantages of the red krypton wavelength. Fig. 10. Advantages and disadvantages of the red krypton wavelength.
|
Less energy is absorbed by the inner retina (see Fig. 8) with decrease of retinal fibrosis. Red light is not absorbed by
yellow macular pigment (xanthophyll). Decreased absorption by
hemoglobin is also useful when treating a deep lesion through a thin
layer of blood in the inner layer of the retina (see Fig. 9). This is true clinically, although theoretically red light is reflected
by the red hemorrhage. Less retinal vasculitis is observed when
treating subretinal structures through or close to retinal blood vessels. The main disadvantage of the red wavelength is that it is absorbed primarily
by melanin in the choroid and pigment epithelium. Variations in
pigmentation will result in unequal energy uptake with similar power settings, creating
the risk of too much irradiance in a small area, which
could result in chorioretinal bleeding. Additionally, the bleeding
is difficult to control with the red laser since the wavelength is not
absorbed by oxygenated hemoglobin (though it is absorbed somewhat
by deoxygenated hemoglobin). Coherent light with an orange wavelength has been obtained with the use
of dye lasers.10 The effect in retinal tissue appears to be a combination of the damage
produced by the yellow and red wavelengths, with much of the damage present
at all levels of the retina. The orange wavelength has never really
been substantially used in the treatment of retinal diseases. The diode laser produces an infrared, long wavelength in the range of 700 to 820 nm. Because
of decreased scattering and absorption, the infrared
laser penetrates vitreous hemorrhage and nuclear sclerotic cataracts
better than shorter wavelengths, such as green and yellow. The deeper
penetration spares the inner sensory retina. The lack of xanthophyll
absorption provides safety of delivery to the macula. The lack of hemoglobin
absorption allows penetration through thin types of pre-retinal
or subretinal hemorrhage without excessive laser energy uptake. Some of the disadvantages of the diode laser include the inability to treat
vascular abnormalities and to adequately treat subretinal neovascular
membranes in light-colored fundi because of lower light absorption. Because
of the higher energy that is usually needed with diode
lasers, a stronger pain response may be elicited (Fig. 11). |
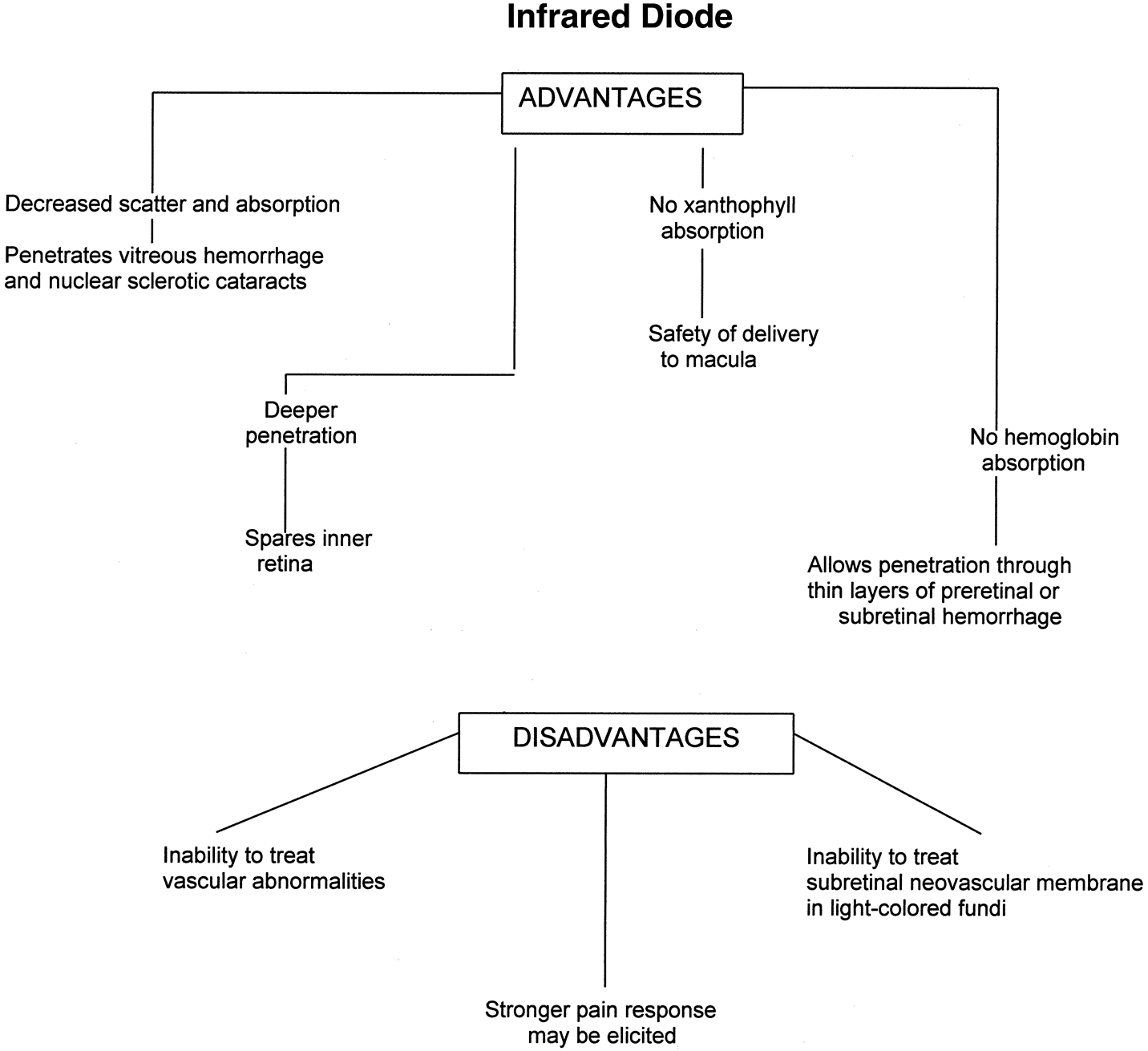 Fig. 11. Advantages and disadvantages of the infrared diode wavelength.
Fig. 11. Advantages and disadvantages of the infrared diode wavelength.
|
The diode laser can be used in direct retinal photocoagulation, transscleral
irradiation, and cycloablative procedures in glaucoma. Additionally, the
diode laser is used for PDT in age-related macular degeneration
and for TTT in occult subretinal membranes. Delivery Systems After a wavelength has been selected, the next question is which system
to use to deliver the laser energy. Delivery systems include the traditional
slit lamp system, endofiber optics for use intraoperatively, the
indirect ophthalmoscope, and contact probes. All ophthalmologists are
familiar with the slit lamp delivery system, which is the most commonly
used. Endolaser photocoagulation is the method in which laser light
is brought directly inside the eye through a fiber optic to apply treatment
to the retina and is only used during vitreous surgery. This
form of treatment is more commonly used than intraocular diathermy, external
cryotherapy, or endodiathermy as a method to produce intraocular
tissue reaction. Binocular indirect ophthalmoscopic laser photocoagulation
has made it possible to treat peripheral retinal lesions that are
unable to be treated by the commercial slit lamp delivery system. This
procedure can be used to treat peripheral retinal tears, proliferative
diabetic retinopathy, and retinopathy of prematurity, to name a few. There are two modes of application of laser energy to tissue: continuous
wave and pulsed. Continuous wave energy is the most commonly used mode
for retinal coagulation because of absorption and the thermal tissue
reaction it produces. Pulsed delivery results in further ablation of
the tissue. The continuous wave laser is produced by excitation of a
gas, which is in a vacuum tube or solid state. The vacuum tube system
has been in use for many years, but is usually larger, less productive, and
depends on a cooling system. Meanwhile, the solid-state system
is smaller, is lightweight, and can be used with an electrical output. Although
it has a limited range of wavelengths, its portability, ease
of use, and size make the solid-state laser the choice of
many ophthalmologists. |