|
At the present time, these IOLs can produce multiple foci using either refractive or diffractive principles. Multifocal IOLs can be constructed, using these principles, in one of several different ways:
- A combination of two or more different anterior spherical refractive surfaces
for distance and near correction
- A combination of an anterior spherical and an anterior aspheric refractive
surface for distance and near correction
- A combination of a posterior spherical refractive surface and multiple
anterior aspheric refractive surfaces
- A combination of an anterior spherical refractive surface and multiple
posterior diffractive structured surfaces for distance and near correction
- A biconvex lens with longitudinal aberrations on the anterior surface (making
it aspheric), providing near vision through the center of the lens, distance
vision through the periphery, and intermediate vision in
between (e.g., the Domilens Progress lens)
OPTICS
Multifocal designs can be classified based on whether they use refractive or diffractive optics to achieve multifocality (Table 1). Diffractive lenses combine an anterior spherical refractive surface with multiple posterior diffractive surfaces.
Table 01. Design Features of Multifocal IOLs
| Design and Model | Manufacturer | Availability | Material | Optics and Features |
| Refractive multifocal | ||||
| Array | Allergan Surgical (Irvine, CA, USA) | Worldwide | Three-piece silicone | Zonal progressive with repeatable, continual power distributions on anterior surface; aspherical; biconvex; distance dominant, 3.5 D add |
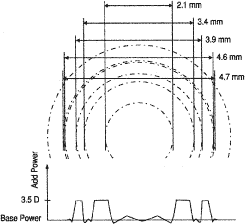
| Domilens Progress 1 | Bausch and Lomb (Claremont, CA, USA) | Europe | One-piece PMMA | Optic diameter of 7.0 mm, Central 4.7 mm anterior surface of progressively increasing power to a final add of +5 D surrounded by an annular distance ring; aspheric; biconvex; near dominant |
| Domilens Progress 3 | Bausch and Lomb (Claremont, CA, USA) | Europe | One-piece PMMA | Same as Progress 1 with 6.5-mm optic diameter and 4.75 D add |
| Refractive bifocal | ||||
| True Vista | Bausch and Lomb (Claremont CA, USA) | Europe | PMMA | Three-zone (central distance, near annulus with 4 D add, peripheral distance); biconvex; distance dominant |
| MF4 | IOLTECH (La Rochelle, France) | Europe | One-piece hydrophilic acrylic | Four-zone (central near with 4 D add, alternating zones of near, distance vision from center); biconvex; near dominant |
| Diffractive bifocal | ||||
| CeeOn 811E | Pharmacia Upjohn (Kalamazoo, MI, USA) | Europe | One-piece PMMA | Bifocal; UV absorbing; concentric diffractive microstructure superimposed on posterior surface of conventional refractive lens; 6.0 mm biconvex optic; 4.0 D add |
| CeeOn 808X | Pharmacia UpJohn (Kalamazoo, MI, USA) | Europe | One-piece PMMA | Same as above with a diameter of 6.5 mm |
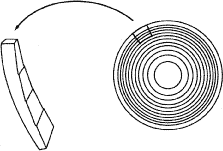
| 3M 825X | Alcon (Fort Worth, TX, USA) | Investigational | Three-piece PMMA | Meniscus-shaped optic; anterior spheric surface with multiple diffraction zones on posterior surface; 4.0 D add |
| 3M 815LE | Alcon (Fort Worth, TX, USA) | Investigational | One-piece PMMA | 27 concentric microslope rings on posterior surface; 3.5 D add |
The mechanism of diffractive lenses is based on the Huygens-Fresnel principle.1 This states that every point of a wavefront can be thought of as being its own source of secondary so-called wavelets, subsequently spreading in a spherical distribution. The amplitude of the optic field beyond this point is simply the sum of all these wavelets. When a portion of a wavefront encounters an obstacle, a region of the wavefront is altered in amplitude or phase, and the various segments of the wavefront that propagate beyond the obstacle interfere and cause a diffractive pattern. A regular array of obstacles that has the effect of producing periodic alterations in the emerging wavefront is termed a diffraction grating. As the spacing between the diffractive elements decreases, the spread in the diffractive pattern increases. By placing the diffractive microstructures in concentric zones and decreasing the distance between the zones as they get further from the center, a so-called Fresnel zone plate is produced that can produce optic foci. Thus the distance power is the combined optic power of the anterior and posterior lens surfaces and the zero order of diffraction, whereas the near power is the combined power of the anterior and posterior surfaces and the first order of diffraction.
Diffraction can be interpreted as a spreading of wavefronts. If the scattered waves are in phase, they interfere constructively; if they are out of phase, they interfere destructively. By assigning appropriate dimensions for the 20 to 30 concentric zones on the posterior lens surface, approximately 41% of the light is in phase and focused for near vision, about another 41% is in phase and focused for distance vision, and the remaining 18% is lost.2 This diffractive optic effect is present at all points (or more precisely, at all sufficiently large areas) of the lens. This means that the multifocal performance of this lens should be unaffected by decentration, pupil eccentricity or deformation, or pupil size; distance and near vision are possible if any part of the lens optic is present behind the pupil.
Conversely, refractive lenses use only differing areas of refractive power to achieve their multifocality. They function by providing annular zones of different refractive power to provide appropriate focus for objects near and far. These lenses may have discrete zones of a near or distant power; thus they may be said to be bifocal. Others may have aspheric surfaces with transition zones resulting in powers that may vary continuously between a minimum for distance and a maximum for the strongest near add. These may be said to be multifocal. Refractive bifocal/multifocal IOLs may be affected by pupil size and decentration, to a greater or lesser degree depending on the size, location, and number of refractive zones. Postoperative pupil size might be a factor of importance in selecting which lens to use. One team investigated whether they could predict postoperative pupil size from preoperative factors.3 They concluded that they could not predict the pupil size with sufficient consistency to ensure a good match between pupil diameter and the zone sizes of various multifocal IOLs.