| Chapter 42 The Optics of Myopia WAYNE G. WHITMORE and BRIAN J. CURTIN Table Of Contents |
|
DEFINITION OF MYOPIA REFERENCES THE ANGLE KAPPA THE CORRECTION OF MYOPIA ANISOMETROPIC MYOPIA VISUAL FIELD ALTERATIONS REFERENCES |
| The optical correction of the myopic eye can present unique and frustrating
management problems. An understanding of the optical considerations
that govern the visual rehabilitation of these patients is indispensable
to their proper management. The prevalence of myopia is about 20% in
the United States population, but varies with age, sex, race, ethnicity, occupation, environment, and other factors in various sampled
populations.1,2 In the average ophthalmic practice, myopes represent an even larger proportion
of patients because of their lifelong dependence on visual aids. Thus, a
thorough understanding of the optics of myopia is essential. The refractive power of the cornea and crystalline lens, modified slightly by anterior chamber depth, determines the refractive power of the eye. In combination with the axial length, these elements determine the refractive state of the eye. Extensive investigations into the range of measurements for these different components of refraction have shown normal distributions for all except axial length. The distribution for axial length shows an excess above the normal random distribution at approximately 23.5 mm and a skew toward increased axial lengths.3 By what appears to be an active process of “emme-tropization,” these components tend to develop and correlate so that most eyes become emmetropic. Animal experiments in primates and other vertebrates have shown that normal postnatal eye growth is dependent on form vision (to the retina) and that with normal development and normal visual input, eyes “seek to become emmetropic.”4,5 |
| DEFINITION OF MYOPIA |
| Myopia is defined as that optical condition of the nonaccommodating eye in which parallel rays of light entering the eye are brought to a focus anterior to the retina. It also can be described as the condition in which the far point of focus is located at some finite distance in front of the cornea. For practical purposes, this is a distance of less than 6 meters, the distance at which visual acuity is normally tested. Thus, the uncorrected, nonaccommodating myopic eye has some point at a finite distance beyond which objects are not seen clearly. At this far point, an object is in clear focus, but with increasing distances beyond it, the image becomes progressively more indistinct (Fig. 1). This far point also is defined as the focal point of the eye. The degree of myopia in diopters is found by determining the reciprocal of the far point or focal point of the eye measured in meters. Therefore, P = I/f where P is the power of the refractive error in diopters and f is the distance of the far point or focal point of the eye in meters from the eye. If thefar point of an eye is at 33.3 cm, then the eye is1/0.333 m = 3.0 D myopic. |
| REFRACTIVE AND AXIAL MYOPIA |
| Myopia can be characterized as refractive or axial, although a continuum of the two types exists. In refractive myopia, the overall refractive power of the eye as determined by cornea and crystalline lens power, modified by anterior chamber depth, is excessive in relation to an eye of normal axial length (21.5 to 25.5 mm). The axial length is normal because it is the product of normal growth. Axial myopia is the result of an excessive elongation of the eye with respect to its refractive components. In these eyes, there is added expansion due to stretching of the scleral wall. These differences in refraction components can have clinical effects. It is of some clinical importance to appreciate that equal amounts of myopic progression are produced by smaller increases in axial length in refractive myopia compared with axial myopia. For example, in refractive myopia, 0.34 mm of axial length change equals approximately 1 D of refractive error change, whereas in axial myopia, 0.4 mm of axial length change equals approximately 1 D of refractive error change.6 The differences between axial and refractive myopia also can affect retinal image size, which is discussed under Image Minification later in the chapter. |
| THE ANGLE KAPPA |
| The angle between the visual and pupillary axes of the eye is defined as the angle kappa. The visual axis in emmetropic eyes is normally slightly medial to the pupillary axis. This is defined as a positive angle kappa. In higher grades of myopia, a temporal shift in the visual axis with respect to the pupillary axis is seen, resulting in a negative angle kappa. Patients with a negative angle kappa may have the illusory appearance of esotropia on cursory examination (pseudoesotropia). This temporal shift of the visual axis in high myopia probably relates to an asymmetric expansion of the posterior segment of the globe. These illusory shifts in the visual axis can be distinguished easily from true tropias by cover testing. |
| THE CORRECTION OF MYOPIA | |||
| The optical correction of myopia with spectacles, particularly the higher
degrees, presents several considerations that must be addressed by
the practitioner. Minus lenses cause image minificationand “barrel” distortion
in addition to prismaticimage displacement. These
problems are more pronounced in larger diameter lenses. Although these
do not present an adjustment problem to myopes accustomed to wearing
spectacles, changes in prescription may bring on their unpleasant optical
effects. The thick-edged lenses necessary for higher myopic corrections
can present cosmetic problems for some patients. These considerations
should be discussed with patients to ease the transition to, and
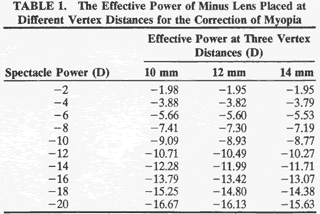
permit a more realistic expectation of their vision with, stronger spectacles. The minus spectacle lens operates at an optical disadvantage when compared with the plus lens, and this is increasingly so with higher degrees of refractive error. As can be seen in Table 1, a minus lens requires substantially greater power to correct a given refractive error than would a plus lens at the same vertex distance. Image minification also becomes more marked with greater lens powers of myopic correction and with increases in lens vertex distance.
Light rays originating from a point more than6 meters in front of the eye are considered for practical purposes to be parallel on entering the pupil. At any point closer to the light source, the rays are said to have vergence, which is measured in diopters. The vergence of a light ray is equal to the reciprocal of its distance, in meters, from its point of origin. Thus, the vergence of light rays at a given point measured in diopters is inversely proportional to the distance from the focal point of those rays. This focal point may be in front of or behind a given reference point, resulting in divergent (i.e., minus vergence) or convergent (i.e., plus vergence) light rays, respectively. The divergence of light rays20 cm from an object of regard with a vergence of-5.0 D is 10 times greater than the divergence of light from the same object at 200 cm with a vergence of -0.5 D (Fig. 2).
A minus lens diverges parallel rays of light. Parallel rays of light entering a -2.0-D lens have a vergence of -2.0 D on leaving the lens, as though the source of the light rays were 50 cm in front of the lens. The optical correction of myopia is accomplished by interposing a minus lens between the cornea and the far (or focal) point of the eye so that the focal point of the lens coincides with the far point (or focal point) of the eye (Fig. 3). The closer the minus lens is placed toward the far point, the stronger it must be. Conversely, the closer the minus lens is placed toward the eye, the weaker the lens required to correct the myopia. To minimize optical disadvantages, the minus lens spectacles should be fitted as close to the eyes as possible. The higher the degree of myopia, the greater the optical benefits of a reduced vertex distance (i.e., the distance between the corneal surface and the lens). It is important to reduce vertex distance when refracting patients with moderate to high myopia (greater than 5 D) and to note this measurement on the spectacle prescription. Minus lens design affects the position of its principal planes. The biconcave lens of equal curvatures has its principal planes between its two surfaces. The meniscus lens, which has one surface convex and the other concave, has its principal planes toward the side of the lens on which the minus power is present. By placing its concave surface toward the eye, the effective vertex distance with the latter type of lens is decreased, which can have definite optical advantages. In the past, meniscus lenses of increasingly stronger base curves had thicker edges, were heavier, produced bothersome image changes, and were cosmetically less acceptable. Newer lenses of higher refractive index, manufactured in both glass and plastic, can now be made in aspheric single vision and aspheric progressive (multifocal) spectacles. Aspheric lenses for myopic corrections have a thinner edge for improved cosmesis and provide superior optics. When viewing through aspheric spectacles off the optical axis, there is less distortion, improved visual acuity, less chromatic aberration, and, in the case with the aspheric surface on the back of the lenses, an enlarged visual field. IMAGE MINIFICATION Figure 4 shows the effect of minus lenses on image size. The angle subtended by the light rays at the nodal point of the eye determines the size of the retinal image. It can be seen that the stronger the correcting concave lens, the smaller the size of the image projected onto the retina. This produces minification of the object. Theoretically, this image minification effect would be more marked in refractive myopia than in axial myopia. Because proportionately stronger minus lenses are needed at greater vertex distances, poorly fitted spectacles with excessive vertex distances increase image minification in the patient with myopia. There is a strong reciprocal relationship between increased vertex distance of spectacle correction and the degree of image minification in myopia (Fig. 5). The ultimate reduction of vertex distance afforded by contact lens correction in the higher grades of myopia results in an increased image size of approximately 20% over that produced by spectacles. The spectacle minification effect for the correction of refractive compared with that of axial myopias can be found in Figure 6. Axial errors are seen to yield small increases in image size with spectacle correction when compared to refractive myopia.7
LENS TILTING To avoid coma, reflections, and image distortion and to accommodate the human facial anatomy, spectacles are best fitted so that the plane of the corrective lenses is perpendicular to the line of sight. Spectacles used for both distance and near are fitted with a downward “pantoscopic tilt” of approximately 7.5 degrees to the visual axis. This represents a compromise of sorts between the visual tasks that involve viewing straight ahead for distance and downward for near. The effect of tilting a minus spherical lens is the production of a minus cylinder at the axis of rotation (180 degrees). The cylindric power increases with both the degree of the tilt and the power of the lens. In addition, there is an increase in the myopic spherical refraction equal to approximately one third of the induced cylindric increase.8 An undercorrected myope is therefore able to obtain better distance acuity by tilting his or her glasses. As an example, the effect of tilt-ing a -10 D lens 10 degrees along the horizontalaxis results in an optical correction of -10.10 -0.31 × 180 degrees with a spherical equivalent of -10.25 D. If this same lens is tilted 30 degrees, the resultant effective optical correction is -10.95 - 3.65 × 180 degrees with a spherical equivalent of -12.78 D. It is not uncommon to see undercorrected myopes tilt their spectacles to attain better distance vision. CONVERGENCE AND ACCOMMODATION If an object of regard is brought toward a fully corrected myope with normal binocular fixation, the increase in divergence of the light rays from the object results in their being focused behind the retina. This stimulates ocular accommodation and convergence so that the image is brought into focus at both foveae. Both accommodation and convergence are altered with the use of minus spectacle lenses. Minus spectacle lenses have the effect of base-in prisms when the visual axes of the eyes are convergent. From Prentice's rule, the amount of prism in diopters is equal to the displacement, in centimeters, from the optical center of the lens times the dioptric power of the lens. P = d × p where P = prismatic power in prism diopters, d = displacement in centimeters from the optical center of the lens, and p = lens strength in diopters. In the case of a bilateral -15 D myope who is looking 3 mm nasal to the optical center of the lens, p = 0.3 × 15, or p = 4.5 prism diopters of inducedbase-in prism in each eye for a total of 9 prism diopters base-in for both eyes. Thus, the convergence required for binocular fixation at near is reduced with minus spectacles. This is a consideration when fitting a high myope with contact lenses who shows a mild degree of convergence insufficiency. Correcting this patient's vision with contact lenses might produce symptoms by increasing the convergence necessary to maintain near vision. The range of accommodation in the uncorrected myope is reduced in nonlinear proportion to the myopic error. This range is defined as the distance from the far point to the near point (i.e., point of focus using maximal accommodation) of the eye and represents the distance over which a clear focus can be achieved. The amplitude of accommodation, conversely, is defined as the difference in the refraction of the eye between these two values expressed in diopters. Figure 7 shows a 16 D range of accommodation in a -4 D myope with and without correction. It can be seen that with correction, the range of accommodation is greatly expanded. Without correction, a myope has the advantage of a closer near point. Thus, for special vocational or avocational needs that demand extended periods of work at a close near point, the removal of glasses often may be advantageous. Medium and high myopes learn of this advantage early in life and instinctively resort to uncorrected near vision for fine, detailed near work. Another maneuver used by many presbyopic myopes is that of sliding their spectacles down on their nose to increase vertex distance. This reduces the effective power of the minus lens and affords better near vision. Spectacle correction with minus lenses also requires less accommodative effort to maintain clear near vision.6 The greater the minus power and the greater the vertex distance of the lens from the eye, the less the accommodation necessary to see a near object clearly. For the hyperope, conversely, the greater the plus power lens and the greater its vertex distance, the greater the accommodative effort required to see an object at the same distance. With correcting spectacles at a vertex of 15 mm, a corrected + 10 D hyperope requires 3.9 D of accommodation to focus on an object 33 cm from his or her eyes, whereas this amount is only 3 D for the emmetrope. A corrected -10 D myope, however, requires only 2.1 D of accommodation to focus on the same object. Clinically, the increased accommodative effort required at near for a spectacle-corrected myope who first starts to use contact lenses frequently induces acute asthenopic symptoms. The possibility of near-vision problems should always be explained carefully to prospective myopic contact lens users, especially those who are approaching presbyopia. BIFOCAL SPECTACLES FOR MYOPIA The base-in prismatic effects of single-vision myopic spectacle lenses at near require modest adjustments in the patient's accommodative-convergence to accommodation ratio (AC/A). Image jump and object displacement due to the presence of two optical centers in bifocals, however, can present formidable adjustment difficulties. As the visual axes are shifted inferiorly and nasally to the optical center of the lenses when reading, both base-down and base-in prisms are induced. The best choice of bifocal lens segments is one that reduces the vertical prismatic displacement. One-piece bifocals, such as the Ultex design, achieve increased positive refraction of their lower segments by a reduction of minus power on the posterior surface of the lens. The optical centers of the lower segment in these lenses are located well below the bifocal line. The base-down prismatic effect in the reading position increases directly with the size and power of the segment. This, combined with the base-down prism of the minus lens carrier, produces an additive effect. Thus, when gaze passes from distant to near objects across the bifocal line, there is a pronounced base-down prism effect with resultant image jump upward and associated object displacement. Both these effects of the Ultex design are usually unacceptable to the wearer. The flat top bifocal, the most widely used bifocal, greatly reduces or almost eliminates these effects. In these bifocals, the optical center of the bifocal segment is located as near as possible to the bifocal line. The truncated circular segments of these bifocals come in sizes of 28 mm, 35 mm, and 45 mm in diameter, with the smaller being the most used. The larger segments have a deeper shelf across the top of the bifocal segment that can make them less attractive. In binocular myopes with roughly equal amounts of refractive error in each eye and who are in the habit of performing some or all of their near work without lenses, the best approach for optical correction often can take the form of avoiding bifocals altogether. A reverse half-spectacle, in which the patient reads below the distance-correcting spectacle, can be an ideal solution. This should always be considered in patients with -2 to -4 D of myopia. PROGRESSIVE ADDITION LENSES Progressive lenses offer a single continuous field of view without the annoying image jump or the disruption of vision by a line across the lens. The disadvantage of these lenses is the astigmatic blurring of images when gaze is directed medially or laterally from the central vertical line of symmetry. The popularity of these lenses is steadily increasing as new presbyopes are being introduced to this type of multifocal. |
| ANISOMETROPIC MYOPIA |
| The optical correction of anisometropic myopia presents the same prismatic
difficulties described above, with additional problems due to the
unequal prismatic effects between the eyes. When gaze is not directed
through the optical centers of unequal myopic spectacle lenses, horizontal
and, more important, vertical phorias or tropias can be induced. Fusional
vergence amplitudes can overcome the effects of these lenses
so that the patient is asymptomatic. At times, however, it may be necessary
for these patients to turn their heads rather than their eyes to
keep the visual axis near the optical centers of the lenses. This is
done instinctively if these situations are presented early in life. Whereas
the anisometropic and presbyopic adult usually has little problem
adjusting to new, carefully centered single-vision reading glasses, the
transition to a bifocal can be a considerable problem. This can be
handled in one of two ways. Different-type bifocal segments with different
locations of their optical centers can be dispensed so that at the
usual reading position, the induced prism between lenses is neutralized. Another
easier method is to reduce the vertical prism induced in
the lower half of a minus lens by eliminating some of the base-down prism
of the stronger lens. This is done by “slabbing off” to
produce a biprism lens. It has the effect of removing a portion of
the base-down prism of the minus carrier lens. Another problem encountered in high anisometropic myopia is that of unequal image minification by the correcting lenses. This can result in sizable amounts of aniseikonia, which can adversely affect binocular vision. Changes in base curve, thickness, and vertex distance of the spectacle lenses can be made to compensate for some of the difference in image size between the two eyes. Contact lenses are the best solution if they can be worn, as they result in the greatest reduction of image size disparity between the two eyes. Because most patients have this problem from birth, neurophysiologic adaptive processes usually facilitate wearing spectacles asymptomatically if they are provided at an early age. Patients who suddenly have a substantial change develop in their spectacle correction, such as from retinal detachment surgery or asymmetric progression of myopia, usually become symptomatic because of aniseikonia. These cases require special consideration when dispensing new spectacles. The ability of many patients, notably children, to fuse in the presence of high degrees of myopic anisometropia may be attributed to “Knapp's rule,” which holds that in axial myopia, correcting lenses placed at the anterior focal plane of the eye produce no change in retinal image size (Fig. 8).9 Regardless of the reason offered, many patients with anisometropic myopia exhibit some grade of fusion while wearing spectacles. It should be clear from all of the forgoing that myopes, especially those with higher errors, need special attention to detail in the selection and fitting of their correcting spectacles. In addition to recording the vertex distance of refraction and the notation of the need for slab-off bifocals, the ophthalmologist should take a moment to advise the patient regarding the choices now available regarding spectacle frame styles and lens types. For example, the patient should know that large frames require large-diameter lenses, which are thicker and heavier, more subject to warpage, and more apt to be dispensed with incorrect lens centration. The thick edges of high minus lenses can be camouflaged to some degree by tinting the lens edges the same color as the frame. Placing the lens further back in the frame by advancing its bevel also is effective in this regard. The use of newer high refractive index lens materials (Table 2) as well as aspheric lens designs allows for more than a 40% reduction in edge thickness and overall weight. Cost may be the only restraint keeping these lenses from being the only ones available on the market today.

Finally, the clinician should always advise the optician to avoid, or at least minimize, any changes in the base curves and thickness of spectacle lenses. If a notable increase in correction is prescribed, necessitating different base curve and lens thickness, it is always best to warn the patient that there may be some difficulty in adjustment to the new spectacles. Some of the effects produced by base curve changes are peripheral distortion, tilting, and increased minification of objects. Head movements accentuate these disturbing visual phenomena, especially peripheral distortion. The patient mayexperience an effect of “floating” and, not infrequently, experience nausea. A moment of explanation can minimize patient concern after new spectacles are obtained. |
| VISUAL FIELD ALTERATIONS |
| While contracting image size, minus spectacle lenses theoretically increase
the visual field. In actuality, this may not be the case because
the thick edges of the minus lenses and the spectacle frame may each produce
peripheral field restriction. The location of the blind spot in
myopic eyes may vary with spectacle correction. The minification of the
visual field should move the blind spot closer to the fixation point. In
clinical practice, however, this effect often is neutralized by
an increase in the distance between the optic nerve and the fovea that
often develops in many myopic eyes. High grades of myopia, in particular, can produce a number of unusual field defects. Concentric contraction occurs occasionally and is thought to be caused by a generalized depression of retinal sensitivity. This field change has been found to occur most often with elevated intraocular pressures. Comet and ring-shaped scotomata somewhat like those seen in glaucoma also are encountered in pathologic myopia. These defects may arise from the sharp, sloping walls of a posterior staphyloma. The sentient retinal elements in this situation are not aligned properly with the pupillary center. A resultant Stiles-Crawford effect with reduced retinal sensitivity results. Hemianopic and quadrantic defects also occur in myopic eyes with posterior staphyloma. These defects are of importance as they may be mistaken as evidence of neurologic disease in those patients who have not had a careful fundus examination. The most common of these defects is bitemporal hemianopsia. This defect is produced by bilateral nasal staphylomas that arise at the optic nerves and involve the fundus areas nasal to it. Most frequently, these staphylomas are inferonasal. The resultant defect is initially relative and is because of ectasia of the affected fundus area. With the subsequent development of chorioretinal degeneration, the visual field will show corresponding absolute defects (Fig. 9). Relative field defects can be eliminated by retesting the affected field with increased minus power to correct for staphyloma depth. CONTACT LENSES The optical benefits of contact lenses over spectacle correction in high myopia include image magnification, the elimination of prismatic object displacement with its attendant “barrel” distortion, and the elimination of image degradation caused by the spherical aberration of spectacle lenses with off-axis viewing (coma).10 As we have observed earlier, when the optical correction in myopia is brought closer tothe corneal surface, image minification decreases. With a contact lens at the corneal surface, image minification is reduced to a minimum. The prismatic effects and spherical aberration of spectacle correctionare eliminated because the optical axis of the contact lens moves with the visual axis of the eye. As noted earlier, the increase in accommodation and convergence effort with the use of contact lenses must be taken into consideration when dispensing lenses. Contact lens technology has advanced significantly in the past decade. Rigid polymethylmeth-acrylate contact lenses have been virtually replaced with daily and extended-wear rigid gas-permeable lenses. Better quality daily and extended-wear toric soft contact lenses are in turn replacing rigid gas-permeable lenses. Many patients who were pre-vious polymethylmethacrylate or rigid gas-permeable contact lens failures can now wear soft contact lenses comfortably. Custom toric soft lenses can correct very high degrees of myopia (up to 20 D at the corneal surface) and astigmatism (up to 10 D at the corneal surface), making comfortable contact lens correction a possibility for most patients. Sufficient patient motivation and normal external ocular anatomy, however, are still essential for successful contact lens wear. Fitting myopes and other patients with high degrees of refractive error, including astigmatism, can be very challenging but also quite rewarding. Refer to a detailed exposition of this subject elsewhere in this text. REFRACTIVE SURGERY The correction of myopia by photorefractive keratoplasty, laser in situ keratomileusis, intrastromal corneal ring implants,11 phakic intraocular lens implants,12 and even clear lens extraction for very high myopia13 have been gaining acceptance among surgeons and patients as the risks for these procedures decrease. With a good surgical outcome and the improvements in medical technology allowing for high-quality optical devices, these methods of optical correction of myopia are superior to spectacle correction by their reduction or elimination of lens aberrations and by their increase in image size relative to spectacle correction. Obviously, the benefits of these methods of optical correction must be weighed against the risks, the downside of which can be considerable. |