Let us see how these basic principles became a practical technique. Regan
and Regan3 and later Regan and Boeder4 outlined the steps in this method of refraction:- Measure the visual acuity with and without the present correction.
- Apply adequate fogging lenses to both eyes.
- Occlude one eye when the blurred vision is static.
- Reduce the fog until the astigmatic axis can be seen.
- Determine the axis on the number 1 astigmatic dial.
- Set a number 2 dial at the determined axis and neutralize with minus cylinders.
- Reduce the sphere to maximal visual acuity.
- (Optional) Remove the cylinder and redetermine the axis on the number 1 dial.
- Refract the fellow eye in the same manner.
- Balance the refraction.
STEPS 1 TO 4 After visual acuity for distance has been measured, the fogging process
is begun. Remember that the patient with normal vision unaided by lenses
probably has little astigmatic error but, if young, may be significantly
hyperopic. In a myope, as previously mentioned, the fog may be
adequate to begin with and may even have to be reduced with minus lenses
to bring the patient's vision to a level suitable for testing
with the dials. In less myopic patients or in hyperopes, sufficient myopia
is simulated and accommodation is relaxed by adding plus spheres
in front of the eye. The end point of the fog is difficult to determine. An old pair of the
patient's spectacles is useful in determining the approximate working
range. Visual acuity is often not a reliable index of the adequacy
of the fog, because acuity varies considerably depending on the degree
of astigmatism. One way of approaching fogging is to continue to add
plus lenses, having the patient close the eyes between changes, until
the denominator of the Snellen notation of visual acuity is doubled (e.g., 20/20 to 20/40 [6/6 to 6/12]).*
Metric equivalent given in parentheses after Snellen notation.Retinoscopy also provides a useful estimate of the proper fog. Neutralize
the most hyperopic or least myopic meridian and place this spherical
correction in front of the eye, being careful not to deduct for the working distance. If retinoscopy is done at 2/3 meter, a
fog of 1.5 diopters (D) will result. Unless large astigmatic errors make it necessary, it is better not to produce
a blur worse than 20/100 to 20/200 (6/30 to 6/90). For the average
patient, a wait of 1 or 2 minutes after fogging induces relaxation
of accommodation. However, in a hyperope who has never worn glasses, 10 or 15 minutes
may elapse before satisfactory relaxation of accommodation
occurs. Once the desired degree of fogging has been induced, the process is reversed
by gradually removing the fogging lenses. As the fog is reduced, watch
carefully for an increase in visual acuity with each decrease in
fogging. If acuity does not increase as expected, attention should be
directed to the astigmatic dial; the astigmatism is probably decreasing
the vision. In a person with 3 or 4 D astigmatism, reducing the fog
by as much as 1 D may not help acuity, although the patient will still
be able to select the axis of astigmatism accurately. STEP 5 If fogging has been correctly performed, enough myopia will have been induced
to suppress accommodation but not enough to impair the intensity
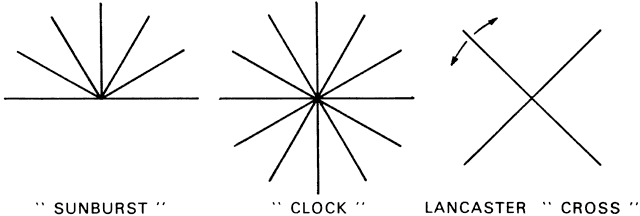
of the black lines on the astigmatic dial. Because it is easier for
a patient to recognize the differing sharpness of radiating lines than
to appreciate differences in visual acuity using letters as test objects, this
is a highly sensitive test for astigmatism. In regular astigmatism, lines
that run in the same direction as the meridian of the greatest
refractive error appear sharply defined. A line therefore appears
sharply outlined when it is accurately refracted in the meridian at
right angles to it. (Another way of stating this is that the clearest
lines are in the axis of least refractive error, the axis closest to
the retina.) Thus, a patient with uncorrected myopic astigmatism at the 180-degree
axis sees the vertical line at the 12- and 6-o'clock positions
most clearly. Make sure the patient's head is not tilted. Superimpose a pointer
over the number 1 chart and ask the patient to select the darkest and clearest lines on the dial and to indicate his or her choice. Hold the pointer
parallel to and alongside the axis you are pointing out, and ask the patient
how many lines on either side of the pointer appear equally dark. Adjust
the pointer to the center of any such group of lines. With larger
degrees of astigmatism (e.g., 2 D), one to three lines are clearer. When astigmatism is small (e.g., less than 1 D), the patient often selects a larger number of lines as
darker or clearer. Sometimes a patient may not discern any difference among the lines on the
dial. If no darker or clearer lines are noted, check the accuracy of
the patient's observations by placing a -0.50 D cylinder at the 90-degree
axis before the fogging lens. The patient should report that
the vertical lines are darker. Likewise, when the cylinder is at the 180-degree
axis, the horizontal lines should come into focus. Often such
a maneuver clarifies what the examiner is testing for and makes astigmatism
apparent for the first time. Now when the cylinder is removed, the
patient can recognize slightly darker or clearer lines on the number 1 dial. STEP 6 Set the number 2 dial so that one line is parallel to the axis determined
previously. This line, of course, appears sharper than the line at
right angles to it. Now introduce minus cylinder in 0.25 D steps with
the cylinder axis parallel to the less dark or less clear line. (A good
way to choose the proper minus cylinder axis is to multiply the lowest
clock hour of the sharp line by 30 degrees. For instance, with a line
running from the 2-o'clock to the 8-o'clock position, 2 × 30 = 60-degree
axis.) Minus cylinder is added until both lines on the number 2 dial
are equally sharp and clear. At this point the patient's
astigmatism has been corrected. The axis of astigmatism may be double-checked by using a Jackson cross
cylinder. The amplitude of astigmatism may be checked by adding -0.25 D
of cylinder first at one axis and then at the perpendicular axis for
comparison. This ensures that the patient sees equally clear lines and
does not require more or less cylinder to equalize the lines. Remember to protect the fog as minus cylinder is added by adding + 0.25 D
of sphere for every 0.50 D of minus cylinder that is given. Protecting
the fog means keeping the astigmatic focal lines in the vitreous
by maintaining the myopic state. If this is not done, the focal lines
may be moved too close to the retina so that the adequate fog is lost
and accommodation is stimulated. STEP 7 When astigmatism has been corrected, reduce the fog in gradual steps. The
goal is to improve visual acuity to 20/15 (6/5) by the least reduction
in sphere that can accomplish this. Remove 0.25 D of fog, and check
the resultant visual acuity. Repeat this procedure until no further
improvement occurs. STEP 8 If desired, the final prescription may be checked by reusing the dials. Removal
of the correcting minus cylinder (the power of which has already
been checked) produces the so-called perfect fog. The posterior focal
line is now on the retina, and refinement of the axis to within 2.5 degrees
is now possible by repeating the use of the dials. STEP 9 Examination of the second eye is done in the identical manner and is facilitated
by the patient's familiarity with the test and the fact
that the examiner has a good idea of what to expect, because most patients
have similar refractive errors in both eyes. STEP 10 Balance the refraction. |